PAYMENT FOR MEDICARE ADVANTAGE PLANS: POLICY ISSUES AND OPTIONS
Office of Health PolicyOffice of the Assistant Secretary for Planning & Evaluation U.S. Department of Health & Human Services
June 2009
The Policy White Papers drafted by the Office of Health Policy (HP) / Office of the Assistant Secretary for Planning and Evaluation (ASPE) describe and analyze key policy issues related to health care financing, public health and health economics. They are intended to provide information that may be useful in policy discussions within these areas. The White Papers may: summarize the issues relevant to key policy topics; provide analysis and evaluation of these issues; provide analysis of policy options and analyze technical/methodological issues related to policy analyses. These papers represent ?working? drafts and may be modified as necessary to respond to new data, new proposals, changes in legislation or regulation, and to public comments.
The Policy White Papers are intended to provide balanced policy analyses and do not advocate specific policy positions or methods. Unless specifically stated, these papers do not represent the positions or policies of the Secretary of Health and Human Services (HHS). Similarly, while any impact or budget estimates presented are made as consistent as possible with current policy baseline estimates, they do not represent official HHS estimates by the Office of the Actuary (OACT).
The paper, ?Payment for Medicare Advantage Plans: Policy Issues and Options,? was prepared by Audrey McDowell and Steven Sheingold under the direction of Dara Corrigan. Nguyen X. Nguyen contributed simulation analyses for evaluating options and Donald Cox contributed to option development. Assistance in preparing budget and enrollment estimates for the options were provided by the Actuarial Research Corporation (ARC) under contract to ASPE. Finally we thank Robert A. Berenson for his review and comments.
This report is available on the Internet at:http://aspe.hhs.gov/health/reports/09/medicareadvantage/
Printer friendly version in PDF format (48 pages) [Free PDF reader  ]
]
Table Of Contents
- Introduction
- Private Health Plans in Medicare: A Brief History
- Medicare Advantage: The Current Landscape
- Evaluating MA Payment and Participation: Overarching Policy Issues
- Specific Issues for Evaluating the Current MA Payment Structure
- The Role and Value of Choices in Medicare
- Should the Medicare Program Pay More for Enrollment in Private Plans Than Would Be the Cost for Comparable Beneficiaries in the Traditional Program?
- Should Payments to MA Plans Equal the Costs of Providing Benefits in the Traditional Program for All Local Markets and Types of Plans?
- Should There Be Pay for Performance in Medicare Advantage?
- Should MA Benchmarks Be Determined by a Competitive Bidding Process?
- Should Traditional Medicare Be Subject to the Competitive Bidding Process?
- The General Context for Considering Policy Options
- Specific Options for Modifying MA Benchmarks
- President?s Budget Option: Competitive Bidding
- Administered Benchmark Option 1: Set County Benchmarks Equal to Local Per Capita FFS Costs
- Administered Benchmark Option 2: Set MA Benchmarks at a Blend of Local and National Average FFS Costs
- Administered Benchmark Option 3: Maintain Current Benchmarks but Modify the Rebate Structure
- Administered Benchmark Option 3a ? Option 3 but Replace the FFS Cost Benchmark with a Blended Benchmark
- Administered Benchmark Option 4 ? Set Local Benchmarks as a Blend of Current Benchmarks and the Average Bid for the Locality
- Concluding Thoughts
- References
List Of Figures And Tables
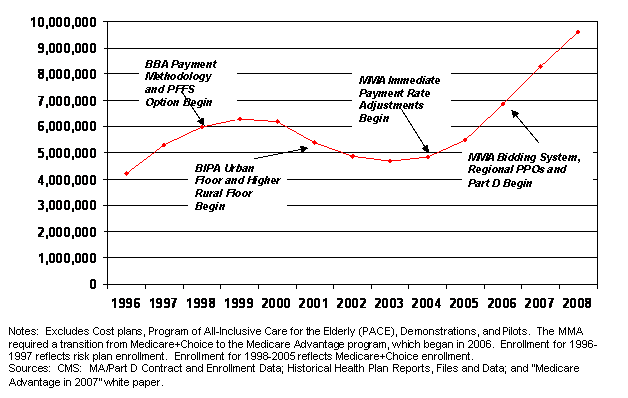
- Figure 1: Historical Trends in Medicare Advantage Enrollment, 1996-2008
- Table 1: Overall Medicare Advantage Penetration, January 2008
- Table 2: Medicare Advantage Plan Availability, 2005-2008
- Table 3: State-Level Availability of Local HMO and PPO Plans, 2006 and 2008
- Table 4: MA Contract, Enrollment, and Plan Counts, By Type, September 2008
- Table 5: MA Enrollment Trends, By Plan Type and County Type, 2005 vs. 2008
- Table 6: FFS Expenditures vs. MA Benchmarks and Payments, By Floor Status, 2006
- Table 7: MA Enrollment Trends, By M+C Program County Payment Type, 2005-2008
- Table 8: MA Enrollment, By Plan Type and Floor Status, 2008
- Table 9: MA Benchmarks, Bids and Payments vs. FFS Expenditures, By Plan Type, 2008
- Table 10: Competing Views on MA Payments
Executive Summary
Medicare Advantage (MA) is the current program under which beneficiaries can enroll in private health plans rather than having their care covered through Medicare?s traditional fee for service (FFS) program. The private plan option has been available in Medicare for over 25 years, during which time the rationale and policy objectives for these plans have evolved. Initially, the basic rationale for private plan participation was that managed care plans could use their provider networks to coordinate high quality care for beneficiaries, provide enhanced benefits, and do so at a cost below that of the traditional fee for service program. The subsequent Medicare + Choice (M+C) program and its successor, Medicare Advantage (MA), were developed with an additional objective in mind ? expanding private plan participation and market competition in Medicare.
In terms of plan choices and enrollment, MA appears to have met with early success. MA enrollment has rapidly grown since 2005 ? currently more than 20 percent of beneficiaries are enrolled in MA. However, the overall structure of the MA program and its value to beneficiaries and taxpayers has been subject to increasing scrutiny and policy debate. Payments to MA plans in many areas are now substantially greater than the cost of treating comparable beneficiaries in the traditional program. The higher payments have raised serious questions regarding Medicare?s fiscal solvency, their net value to the program and their equity implications for beneficiaries.
These issues have resulted in considerable debate in recent years concerning whether to maintain MA rates at current levels or whether to reduce them to levels commensurate with the cost of comparable beneficiaries in the traditional fee for service program. In structuring possible alternatives, and in choosing among them, it is useful to consider several policy issues:
- Whether maintaining choices among competing private plans is the best option for improving value and financial sustainability within the Medicare program;
- Whether the Medicare program should ever pay more in aggregate for enrollment in private plans than would be the cost for comparable beneficiaries in the traditional program, and if so, under what conditions;
- Whether payments to some MA plans should ever be higher than the costs of providing benefits in the traditional program even if budget neutral in aggregate
- Whether there should be pay for performance in Medicare Advantage; and
- Whether MA benchmarks should be determined by a competitive bidding process.
Views and positions of on these issues can be considered within the context of longer term debates concerning the role of government versus private markets in health policy, and the role of private plans and competition in Medicare. Nonetheless, if policymakers decide to modify payments in order to achieve budget savings, induce greater competition, or both, there would be a number of options available.
Currently, payments to individual MA plans are determined by county level benchmark amounts, each plan?s bid, and a rebate structure. Specifically, plans whose bids are below the county benchmark receive their per capita bid risk adjusted for each enrollee, plus a rebate equal to 75 percent of the difference between the bid and the benchmark. Plans bidding above the benchmark amount receive a risk adjusted per capita payment equal to the benchmark and generally must charge a supplemental premium to beneficiaries.
For a number of reasons, moving away from administered benchmarks to ones set through a competitive bidding process would be a preferred method for modifying current payments. Most importantly, a well-functioning bidding process should result in benchmarks that would better reflect the costs of providing high-value care within the local markets. In the past, however, health plans and their supporters have resisted such a bidding approach. In addition, there are a number of important policy questions to address with regard to the exact structure of the bidding process and potential competition with the traditional program. Thus, options might be considered in the short run that could represent a transition from administered benchmarks to a competitive pricing system in a way that reduced payments relative to current law and provided increasing incentives for market competition among MA plans. These options might be structured to modify the current benchmarks, modify the rebate structure, or both. In this paper we describe and analyze five such options for modifying MA payment rates:
- Option 1: Set
County
Benchmarks Equal to Local Per Capita FFS Costs - Option 2: Set MA Benchmarks at a Blend of Local and National Average FFS Costs
- Option 3: Maintain Current Benchmarks but Modify the Rebate Structure
- Option 3a: Option 3 but Replace the FFS Cost Benchmark with a Blended Benchmark
- Option 4: Set Local Benchmarks as a Blend of Current Benchmarks and the Average Bid for the Locality
All of these options would reduce payments to MA plans substantially and are estimated to result in significant reductions in MA enrollment relative to baseline projections. Estimated spending reductions range from 7.5 percent for Option 3 to over 12 percent for Options 1 and 2. There would also be differences in terms of impacts on different localities and types of MA plans. For purposes of this analysis, it was assumed that the first year of implementation for each option would be 2011, and that all policy changes would be fully implemented during that year. If the changes were implemented on a phased basis, then the impacts would be spread out over a larger number of years, and the projected amount of short-term savings would be smaller.
[ Go to Contents ]
Introduction
Medicare Advantage (MA) is the current program under which beneficiaries can enroll in private health plans rather than having their care covered through Medicare?s traditional fee for service (FFS) program. The private plan option has been available in Medicare for over 25 years, during which time the rationale and policy objectives for these plans have evolved. Initially, the basic rationale for private plan participation was that managed care plans could use their provider networks to coordinate high quality care for beneficiaries, provide enhanced benefits, and do so at a cost below that of the traditional fee for service program. The subsequent Medicare + Choice (M+C) program and its successor Medicare Advantage (MA), which began in 2006, were developed with an additional objective in mind ? expanding private plan participation and market competition in Medicare. It was hoped that providing a greater number and variety of plan choices to beneficiaries would spur competition between plans, and eventually between private plans and the traditional program, in a way that would introduce efficiency and cost savings in Medicare.
In terms of plan choices and enrollment, MA appears to have met with early success. MA enrollment has rapidly grown since 2005 ? currently more than 20 percent of beneficiaries are enrolled in MA.[1] Moreover, enrollment has increased rapidly in geographic areas where there previously was less participation, such as in rural areas. Recently, enrollment has also increased rapidly in private fee for service plans, an alternative to the original coordinated care plans.
However, the overall structure of the MA program and its value to beneficiaries and taxpayers has been subject to increasing scrutiny and policy debate. Payments to MA plans in many areas are now substantially greater than the cost of treating comparable beneficiaries in the traditional program. The implications of these higher payments for Medicare?s fiscal solvency, as well as the equity implications for beneficiaries, have been of concern. There are also questions regarding whether there are additional benefits to MA that are commensurate with the extra spending. To date, quality of care has been found to be comparable between MA and traditional fee for service. While MA plans do provide additional covered services and/or reduced cost-sharing, the equity aspects of having these additional benefits partially financed by beneficiaries remaining in the traditional program[2] are clearly controversial. These issues have resulted in a number of proposals that would reduce payments to MA plans or restructure the process for determining those payments.
In this paper, we provide a detailed description of the MA program, describe the issues related to the MA payment debate, and analyze options that might be considered for modifying the current methods of determining MA payment amounts.
[ Go to Contents ]
Private Health Plans in Medicare: A Brief History
Medicare?s ability to offer private health plans as options for beneficiaries began with the Social Security Amendments of 1972, which authorized risk contracting with managed care plans. However, it was not until changes made in the risk sharing arrangements under the Tax Equity and Fiscal Responsibility Act (TEFRA) of 1982 that plan participation and enrollment began to increase. TEFRA introduced the policies of administered pricing for plan payments and of allowing plans to provide beneficiaries with additional benefits and/or reduced cost sharing. It also introduced assured savings for the program by paying 95 percent of the estimated cost of treating an average beneficiary in the traditional fee for service (FFS) program (the adjusted average per capita cost (AAPCC)). Health maintenance organizations (HMOs) contracted with Medicare to provide the full range of Medicare Part A and Part B benefits, and received a monthly capitation payment per enrollee. Enrollment grew to about 6 million beneficiaries by 1997, primarily concentrated in urban counties.
The Balanced Budget Act of 1997 (BBA) renamed the private health plan program as Medicare+ Choice (M+C) and made significant changes. First, in order to build on changes in the private insurance markets, the BBA allowed several new types of plans, including: private fee for service plans (PFFS), preferred provider organizations (PPOs), and Medicare medical savings account plans (MSAs). Second, the BBA revised payment formulas for private plans by setting national payment floors for lower cost counties and guaranteeing a minimum 2 percent annual increase to all plans.[3] The BBA also authorized the Secretary to implement a risk adjustment to the payment rates based on enrollees? health status.
The payment mechanism implemented under M+C weakened the linkage between private plan payment rates and FFS costs, and for the first time resulted in plan payments in some areas being higher than the costs of treating similar patient in the traditional fee for service program. The net result of all of the BBA changes, however, was that M+C enrollment began to decline rapidly. The increase in payment rates for rural areas was not sufficient to attract increased participation. Meanwhile, plans in many of the localities with the greatest M+C enrollment were limited to the two percent annual increases in the premiums paid by the program at a time when health care costs began to rise much more rapidly. As a result, by 1999, many plans began to withdraw from the program and enrollment fell from its peak of 6.3 million in 1999 to 5.4 million in 2001.
The Benefits Improvement and Protection Act of 2000 (BIPA) attempted to stop the decline in the program by increasing the national payment floor, creating a second higher urban floor, and increasing the minimum payment update from March 2001 through the end of the calendar year. However, enrollment in private plans continued to decrease, falling to 4.7 million by 2003.
Medicare Advantage (MA) was authorized under the Medicare Prescription Drug, Improvement, and Modernization Act of 2003 (MMA) (P. L. 108-173) as a successor to M+C. The MMA, which was enacted on December 8, 2003, was intended to reverse the downward trend in Medicare private health plan enrollment by providing immediate enhancements to MA plan payment rates (such as a 6.3 percent minimum update for 2004) and other program improvements that were designed to encourage plan participation. The MMA expanded Part C to include both local MA plans and a new MA regional plan option,[4] and beginning in 2006, the MMA required the MA program to begin using a new competitive bidding process for both local MA and regional MA plans.[5] The MMA also authorized MA special needs plans (SNPs), which target three specific subsets of the beneficiary population: those who are institutionalized, dually eligible; and/or have severe or disabling chronic conditions. Additionally, beginning in 2006, MA plans offering integrated Part D prescription drug coverage (MA-PDs) became available under the new voluntary Medicare prescription drug benefit.
Medicare private plan enrollment has historically been sensitive to changes in payment policy (see Figure 1), which can affect plan participation and benefit design.
Figure 1: Historical Trends in Medicare Advantage Enrollment, 1996-2008
Despite some initial uncertainty about how many insurers would participate and how many beneficiaries would take up the coverage, there seems to have been a significant response to the changes that were made under the MMA. Private plan enrollment has increased significantly, with more than a fifth of all Medicare beneficiaries enrolled in MA plans (9.8 million, or 21.7 percent as of September 2008).
As discussed below, there has been considerable concern that payment rates for MA plans are too high relative to the costs of caring for comparable beneficiaries under the traditional FFS program. The Medicare Improvements for Patients and Providers Act of 2008 (MIPPA) provided for a small reduction in MA payments by phasing out of the inclusion of indirect medical education (IME) costs in the calculation of MA payment rates. MIPPA also included a provision that is expected to slow the growth in PFFS enrollment: a requirement that all employer-sponsored PFFS plans, as well as all non-employer sponsored PFFS plans in areas with at least two other MA plans that have provider networks, develop written provider contracts beginning in 2011.[6] MIPPA also directed the Medicare Payment Advisory Commission (MedPAC) to study the relationship between MA plan bids and county level FFS costs, identify alternate MA payment approaches, and submit a report to Congress in March 2010.[7]
[ Go to Contents ]
Medicare Advantage: The Current Landscape
Types of Medicare Advantage Plans
The MA program offers a continuum of plan choices that range from fee-for-service (the most loosely managed) to health maintenance organizations (the most tightly managed), and include many features that are comparable to what is available in the commercial market. The following is a brief overview of the major types of MA plans that are currently available.[8]
- Local Coordinated Care Plans (CCPs) primarily consist of Local Health Maintenance Organizations (HMOs), which have defined provider networks and primary care gatekeepers; and Local Preferred Provider Organizations (PPOs), which are characterized by defined provider networks, no requirement that beneficiaries obtain referrals for specialty care, and higher cost-sharing requirements for out-of-network services.
- Regional Coordinated Care Plans (CCPs) consist of Regional PPOs, which have a State-level service area (consisting of one or more of 26 State-level or Multi-State CMS-defined regions), combined Part A / Part B deductible, and an annual catastrophic limit on Part A / Part B cost-sharing.
- Private Fee-For-Service Plans (PFFS) are local plans that are not required to have a contracted provider network (until 2011) as long as they pay willing providers based on Medicare FFS rates. They are exempted from reporting quality data (until 2010).
- Medicare Medical Savings Account Plans (MSA) are local plans that offer a high-deductible health plan that is linked with a medical savings account.[9] Medicare MSA plans are required to offer a benefit package that is actuarially equivalent to traditional Medicare?s benefit package, and to cover 100 percent of beneficiaries? Medicare-covered services once the enrollee has met the annual deductible (which can be no higher than $10,500 in 2009). Enrollees in MSA plans are allowed to access any Medicare-certified provider; however, MSA plans are also allowed to have preferred provider networks. Unlike other MA plans, MSA plans? bids are not subject to CMS review (Fuchs, 2007). These plans are also exempted from reporting quality data (until 2010).[10]
- Special Need Plans (SNPs) are local or regional MA plans that target one of the following subsets of the beneficiary population: those who are dually eligible (Medicare/ Medicaid), those who have chronic or disabling conditions, or those who are institutionalized. MIPPA extended the authorization for SNPs through 2010 and added some additional enrollment, care coordination, and quality reporting requirements.
- Employer Group Waiver Plans (EGWP or 800 series plans) are MA plans that target the employer/union group market (rather than the individual market), and for which CMS has waived some of the general requirements that apply to MA plans. They include Employer Direct plans, in which the employer/union contracts directly with CMS to offer a MA plan to their Medicare-eligible retirees; and Insurer-Sponsored plans in which the employer/union contracts with an insurer that is offering a MA group product that can be tailored to meet their particular needs.
With the exception of MSA plans, all MA plans have the option of offering integrated Part D coverage. MA plans that offer Part D coverage are known as MA-PD plans, while MA plans that do not offer Part D coverage are known as MA-Only plans.
[ Go to Contents ]
General Requirements For Medicare Advantage Plans
MA plans are statutorily required to meet several key requirements. However, there are some important differences in requirements by plan type.
- Actuarial Equivalence ? MA plans are required to offer a benefit package that is actuarially equivalent to traditional Medicare?s benefit package (e.g. having the same value, based on the estimated spending that would be incurred by the insurer). MA plans are required to cover at least all of the medically-necessary services (e.g., Part A and Part B benefits) that are covered under the FFS program, but they are allowed to charge different copayments, coinsurance, and deductibles, as long as the benefit design does not discriminate against sicker beneficiaries. Note: Regional PPOs are also required to offer a combined A/B deductible and an annual limit on A/B cost-sharing. Although MSA plans are allowed to offer a high-deductible health plan that is linked to a Medicare medical savings account into which the plan makes an annual contribution, these plans are still required to meet actuarial equivalence requirements.
- Service Area ? MA plans are required to only enroll beneficiaries who live in their defined geographic service area, which is determined by the MA organization, and submitted to CMS for approval. MA organizations are allowed to offer multiple MA ??plans?? (e.g., benefit designs) that have the same service area under a single MA ?contract.? They can also submit requests for service area expansions and reductions. Note: Local MA plans can define their service area to consist of one or more counties, with no requirement that the counties be contiguous, and also have the option of requesting CMS approval to include partial counties in their service area. However, regional MA plans are required to include one or more of the 26 CMS-defined State-level or multi-State regions in their service area.
- Uniform Benefits ? MA plans must offer uniform benefits, premiums and cost-sharing arrangements to all beneficiaries residing in the plan?s service area. Note: Local plans are allowed to have segmented service areas, where benefits, premiums, and cost sharing can vary across segments comprised of one or more MA payment areas (e.g., counties). MA organizations are required to submit a separate bid for each segment.
- Access ? MA organizations are required to ensure that covered services are ?available and accessible? within the plan?s geographically defined service area. CMS reviews the plans? written provider contracts and provider networks for network adequacy. Plans are also required to cover urgently-needed services beyond service area. Note: Prior to the enactment of MIPPA, PFFS plans were allowed to meet the access requirement through deeming.[11] However, MIPPA requires that most PFFS plans develop contracted provider networks starting in 2011.
- Guaranteed Issue ? MA organizations must offer a given MA plan to all eligible individuals in the service area, and enroll any eligible service area resident who elects the plan during an applicable enrollment period.[12] Note: Employer/Union group waiver plans (EGWPs) and Special Needs Plans (SNPs) are allowed to limit enrollment to a subset of the eligible beneficiary population.
- Reporting of Quality Data ? MA plans are required to submit several types of data on quality measures, including: Healthcare Effectiveness Data and Information Set (HEDIS), Consumer Assessment of Healthcare Providers and Systems (CAHPS), and Health Outcomes Survey (HOS). Note: The MMA exempted PFFS and MSA plans from reporting quality data. The MMA also required PPOs to submit less data on HEDIS measures than HMOs (PPOs are not required to report on the services of out-of-network providers, or on measures that are based on data that have been extracted from medical records). However, MIPPA requires PFFS plans to report the same quality data as PPOs beginning in 2010.
- Marketing ? MA plans must adhere to the CMS Medicare Marketing Guidelines, including submission of marketing materials and website content to CMS for review and approval. Additionally, CMS recently published several regulations relating to new marketing provisions for the Fall 2008 open enrollment period, including a MIPPA requirement to establish guidelines to ?ensure that the use of compensation creates incentives for agents and brokers to enroll individuals in the Medicare Advantage plan that is intended to best meet their health care needs.?
[ Go to Contents ]
Payment Methods for Medicare Advantage Plans
The MMA created a new competitive bidding process for MA plans. Beginning with the 2006 contract year, MA organizations are required to submit bids to provide coverage to beneficiaries in their defined service area (or segment). MA plans submit separate bids to CMS for Part A and Part B services, and for Part D benefits (if offered). These bids are then compared to pre-set county level benchmarks in order to determine payments to plans.
Determination of Payments for Part A and B Services
Under the statutorily mandated competitive bidding process, monthly capitation payments to MA plans are determined by a combination of: 1) the relationship between plans? bids and the appropriate county or regional ?benchmarks? (bidding targets), and 2) the enrolled beneficiaries? demographics and health risk characteristics (risk-adjusted based on the Hierarchical Condition Categories (HCC) model).
MA organizations are required to submit bids to CMS based on the expected cost of providing coverage to an average Medicare beneficiary. The bid for Part A/B services includes costs for services, administrative costs, and a projected surplus or profit, and excludes cost sharing that beneficiaries would pay under traditional Medicare Parts A and B.
In order to determine the payment for each plan, the bids for Part A and Part B services are compared with local (county level) or regional MA benchmarks. If a plan bids above the benchmark, then the plan receives a base rate that is equal to the benchmark, and the enrollees must pay an additional premium equal to the difference between the bid and the benchmark. If a plan bids below the benchmark, it receives a base rate equal its bid plus a rebate that is equal to 75 percent of the difference between its bid and the benchmark. The plan must return the rebate to enrollees in the form of supplemental benefits or lower premiums.[13]
How the local MA benchmarks for Part A and B services are set.
CMS calculates local county-level benchmarks based on historical county-level MA payment rates, adjusted for growth in Medicare spending, or estimated FFS costs.[14]
Under the MA program, the benchmark in a given county is the greater of: 1) the estimated average FFS costs in the county for the year (excluding direct GME), or 2) the payment rate set for the county in the previous year, updated for expected national average growth in Medicare spending based on the ?minimum percentage increase? (which is defined as the growth in national per capita Medicare spending).[15] [16] For local MA plans serving multiple counties, the benchmark is the weighted average of the individual county benchmarks, based on the expected geographic distribution of the plan?s enrollees.
How the regional MA benchmarks for Part A and B services are set. Unlike the local benchmarks, which are set solely based on administrative data (such as historical county-level rates), CMS determines the regional benchmarks by combining the average county rate and the average plan bid for each State-level or multi-State region. The regional benchmark represents the sum of the following two components ? the ?statutory component,? which is the weighted average of the local (county) benchmarks in the region, and the ?plan bid component,? which is the weighted average of regional plan bids in the region. The relative weights of the plan bid and statutory components in the formula are determined based on the national proportion of MA-eligible beneficiaries who were or were not enrolled in an MA plan, respectively. Thus, as the national MA market share increases, the ?plan bid component? (e.g., the weighted average of plan bids) will account for a larger share of the regional benchmarks.[17]
Impact of payment floors on MA benchmarks. The pre-2006 county-level MA payment rates that serve as the basis for current MA payments often exceeded comparable average per capita FFS Medicare costs. As discussed earlier, this is in part because over the past decade, Congress has set payment floors to stimulate plan growth in rural areas. For example, the BBA (1997) created a national payment floor, and BIPA (2000) increased the national floor rate and created a second, higher urban floor rate for counties located in Metropolitan Statistical Areas (MSAs) with at least 250,000 people. As discussed below, these floors have increased county benchmarks to well above local FFS costs.
Determination of Payments for Part D Services
CMS calculates the payment for the Part D portion of the MA plans? benefits (if offered) separately. All plans offering the Medicare Part D prescription drug benefit (including both MA-PDs and standalone Prescription Drug Plans) submit bids to CMS based on the expected cost of providing Part D coverage to an average Medicare beneficiary.
CMS calculates a nationwide average bid based on all of the plans? standardized bid amounts for basic coverage. Enrollees pay a base premium, plus any difference between their plan?s bid and the nationwide average bid. CMS pays each plan a monthly prospective capitation payment for each enrollee (adjusted based on the enrollee?s risk weight) and other factors, with a final reconciliation based on actual data after the end of each year. Plans can receive additional payments for low-income subsidy (LIS) enrollees, reinsurance costs, and risk sharing. CMS updates the deductible, initial coverage limit, and catastrophic threshold amounts for the standard Part D benefit each year, based on the estimated annual change in per capita drug spending.
Many MA-PD plans use a portion of the rebate dollars that they receive for bidding below the relevant benchmark for Part A and B services to reduce the premium for Part D services. As a result, in 2008, the average MA-PD enrollee paid a $13 Part D premium, while the average enrollee in a standalone prescription drug plan paid a $32 Part D premium. During that year, 88 percent of all beneficiaries had access to at least one MA-PD plan that offered a zero premium for Part C and Part D coverage[18] (MedPAC, 2008a).
[ Go to Contents ]
Recent Trends in Medicare Advantage Plan Participation and Enrollment
More than one in five of the nation?s 44 million Medicare beneficiaries were enrolled in MA plans as of January 2008 (see Table 1).
Table 1: Overall Medicare Advantage Penetration, January 2008
| Note: Some numbers may not add to totals due to rounding. By September 2008, MA penetration had increased to 21.7 percent (9.8 million enrollees). | ||
| Source: CMS January 2008 Enrollment Data and Press Release | ||
| Description | Enrollment | % of Total |
| Total Medicare Beneficiaries(excludes those living outside of a MA service area, in prison, etc.) | 44.1M | 100% |
| Original Medicare Enrollment (Fee For Service) | 34.7M | 79% |
| Total Medicare Advantage Enrollment | 9.0M | 20% |
| Other Private Plan Enrollment (Cost Plans, PACE, Demonstrations, Pilots) | 0.4M | 1% |
As discussed later in this section, the increase in MA enrollment that has occurred during recent years has resulted from greater plan participation across geographic areas and the enhanced benefits they are able to provide under the current MA payment structure.
Plan Availability
As discussed earlier, one of the objectives of the MA program was to provide a greater number and variety of plan choices to beneficiaries as a way of expanding private plan participation and market competition in Medicare. In 2003, only 58 percent of beneficiaries had access to a M+C plan, down from 74 percent availability in 1998 (MedPAC, 2003). However, the MMA?s immediate payment rate adjustments encouraged plans to enter or reenter the market and/or expand their service areas, so that by the time that the MA program began in 2006, 100 percent of beneficiaries had access to at least one MA plan. Since then, the average number of plans available to beneficiaries has continued to increase (see Table 2).
Table 2: Medicare Advantage Plan Availability, 2005-2008
| Source: MedPAC March 2008 Report to Congress | ||||
| Type of Medicare Advantage Plan | 2005 | 2006 | 2007 | 2008 |
| Local Coordinated Care Plans (CCPs - HMOs and PPOs) | 67% | 80% | 82% | 85% |
| Private Fee For Service Plans (PFFS) | 45% | 80% | 100% | 100% |
| Regional Coordinated Care Plans (CCPs - PPOs only) | N/A | 87% | 87% | 87% |
| Medicare Medical Savings Account Plans (MSAs) | 0% | 0% | 77% | 100% |
| Total - All Medicare Advantage Plan Types | 84% | 100% | 100% | 100% |
| Average Number of MA Plans Open to All Beneficiaries in a County | 5 | 12 | 20 | 35 |
In 2008, 100 percent of beneficiaries had access to a PFFS plan or an MSA plan, and most beneficiaries had access to a Local HMO or PPO (85 percent) or a regional PPO (87 percent).
However, the widespread national availability of various types of MA plans masks some State-level and regional discrepancies. For example, only 43 percent of rural beneficiaries had access to a Local HMO choice, and only 32 percent had access to a Local PPO choice in 2008.
Additionally, there were five States that did not have any Local HMO plan choices in 2008, and an additional 17 States where 25 percent or more of beneficiaries did not have access to a Local HMO. Many of these States with low Local HMO plan availability also did not have extensive availability of Local PPO choices (see Table 3). There were only 4 States in which all rural beneficiaries had access to a Local HMO choice, and an additional 11 States in which more than half of the rural beneficiaries had access to at least one Local HMO (Gold et. al., 2008).
Table 3: State-Level Availability of Local HMO and PPO Plans, 2006 and 2008
| Source: Gold et. al., 2008 | |||||||
| Category | State | 2006 | 2008 | ||||
| Percent of Beneficiaries With One or More Choices: | Percent of Beneficiaries With One or More Choices: | ||||||
| Local HMO | Local PPO | Regional PPO | Local HMO | Local PPO | Regional PPO | ||
| Total, All States | 72% | 63% | 88% | 80% | 63% | 88% | |
| States Where 0% of Beneficiaries Had 1+ HMO Choices in 2006 | Alaska | 0% | 0% | 0% | 0% | 0% | 0% |
| Delaware | 0% | 0% | 100% | 54% | 0% | 100% | |
| Maine | 0% | 44% | 0% | 79% | 56% | 0% | |
| Montana | 0% | 71% | 100% | 23% | 71% | 100% | |
| North Dakota | 0% | 0% | 100% | 0% | 0% | 100% | |
| South Dakota | 0% | 0% | 100% | 0% | 2% | 100% | |
| Vermont | 0% | 0% | 0% | 0% | 0% | 0% | |
| Wyoming | 0% | 0% | 100% | 3% | 0% | 100% | |
| States Where 1% - 25% of Beneficiaries Had 1+ HMO Choices in 2006 | Indiana | 4% | 39% | 100% | 44% | 39% | 100% |
| Virginia | 16% | 57% | 99% | 36% | 63% | 100% | |
| Mississippi | 18% | 0% | 100% | 61% | 0% | 100% | |
| South Carolina | 23% | 47% | 100% | 32% | 58% | 100% | |
| States Where 26% - 50% of Beneficiaries Had 1+ HMO Choices in 2006 | New Hampshire | 27% | 0% | 0% | 0% | 0% | 0% |
| West Virginia | 28% | 100% | 100% | 35% | 100% | 100% | |
| Arkansas | 30% | 0% | 100% | 76% | 51% | 100% | |
| Nebraska | 32% | 0% | 100% | 33% | 31% | 100% | |
| Kansas | 35% | 30% | 100% | 41% | 39% | 100% | |
| Kentucky | 35% | 38% | 100% | 36% | 39% | 100% | |
| Georgia | 41% | 45% | 100% | 52% | 45% | 100% | |
| Louisiana | 49% | 46% | 100% | 89% | 24% | 100% | |
| New Mexico | 49% | 100% | 0% | 69% | 100% | 0% | |
| States Where 50% - 75% of Beneficiaries Had 1+ HMO Choices in 2006 | Oklahoma | 52% | 63% | 100% | 62% | 63% | 100% |
| Idaho | 56% | 70% | 0% | 83% | 78% | 0% | |
| North Carolina | 56% | 41% | 100% | 67% | 56% | 100% | |
| Utah | 61% | 87% | 0% | 92% | 89% | 0% | |
| Missouri | 63% | 65% | 100% | 68% | 67% | 100% | |
| Texas | 67% | 55% | 100% | 79% | 55% | 100% | |
| Iowa | 68% | 22% | 100% | 78% | 47% | 100% | |
| Wisconsin | 71% | 48% | 100% | 78% | 52% | 100% | |
| Michigan | 73% | 50% | 100% | 84% | 56% | 100% | |
| Alabama | 74% | 57% | 100% | 58% | 100% | 100% | |
| States Where 75% - 100% of Beneficiaries Had 1+ HMO Choices in 2006 | Illinois | 76% | 88% | 100% | 77% | 88% | 100% |
| Maryland | 79% | 79% | 100% | 84% | 84% | 100% | |
| Tennessee | 82% | 68% | 100% | 88% | 56% | 100% | |
| Colorado | 84% | 63% | 0% | 81% | 63% | 0% | |
| Washington | 87% | 78% | 0% | 94% | 91% | 0% | |
| Minnesota | 88% | 0% | 100% | 100% | 0% | 100% | |
| Ohio | 88% | 89% | 100% | 100% | 90% | 100% | |
| Nevada | 89% | 100% | 100% | 89% | 100% | 100% | |
| Florida | 90% | 78% | 100% | 97% | 81% | 100% | |
| Arizona | 92% | 81% | 100% | 92% | 86% | 100% | |
| California | 93% | 41% | 100% | 93% | 8% | 100% | |
| New York | 93% | 99% | 100% | 95% | 100% | 100% | |
| Oregon | 93% | 100% | 0% | 93% | 100% | 0% | |
| Pennsylvania | 95% | 95% | 100% | 96% | 100% | 100% | |
| Massachusetts | 97% | 97% | 0% | 97% | 97% | 0% | |
| Connecticut | 100% | 75% | 0% | 100% | 81% | 0% | |
| District of Columbia | 100% | 100% | 100% | 100% | 100% | 100% | |
| Hawaii | 100% | 77% | 100% | 100% | 72% | 100% | |
| New Jersey | 100% | 87% | 100% | 100% | 87% | 100% | |
| Rhode Island | 100% | 86% | 0% | 100% | 0% | 0% | |
Plan Participation
As of September 2008, there were a total of 612 MA contracts and 4,467 MA plans (benefit designs). On average, there were about 7 MA plans per contract. Local CCPs (including HMOs and PPOs) accounted for most of the MA plans (73 percent), followed by PFFS plans (22 percent). Approximately 17 percent of the MA plans were SNPs, and nearly a quarter of the MA plans (24 percent) were only open to Employer Group members. Additionally, nearly three-quarters of all MA plans (74 percent) offered integrated Part D coverage (see Table 4).
Enrollment By Plan Type
As of September 2008, most of the nation?s 9.8 million MA enrollees were in Local CCPs (e.g., HMOs and PPOs, 73.5 percent) or PFFS plans (23.4 percent). Regional PPOs accounted for only 3 percent of the MA enrollees that year, and fewer than 1 percent were enrolled in Medicare MSA plans (see Table 4).
Most of the MA enrollees were in MA-PDs (85 percent). Additionally, more than 1 in 10 MA enrollees were in Special Need Plans (13 percent, including 9 percent who were in Dual-Eligible SNPs), and nearly 2 in 10 MA enrollees (17 percent) were in Employer Group Waiver Plans.
Total 2008 MA enrollment compares favorably with the enrollment projections that were included in the regulatory impact analysis for the program (9.33 million). However, while the impact analysis had assumed that 33 percent of the enrollees would be in the newly created Regional PPO plans (3.1 million), much of the actual growth has occurred in PFFS plans.
Table 4: MA Contract, Enrollment, and Plan Counts, By Type, September 2008
| Notes: Numbers may not add to totals due to rounding. (1) MA-PD contract count represents the number of contracts including at least one MA-PD. (2) SNP information is based on the Special Needs Plan Comprehensive Report. Non-SNP information represents the difference between the MA total and the SNP subtotal. SNP contract counts represent the number of contracts including at least one SNP plan. (3) Employer Group contract counts represent the number of contracts including at least one employer group plan. | ||||||
| Source: CMS September 2008 Enrollment Data | ||||||
| Description | Contracts | Enrollment | Plans | |||
| Number | % of Total | Number | % of Total | Number | % of Total | |
| Total - All Medicare Advantage Plans (excludes Cost, PACE, Demos, Pilots) | 612 | 100.0% | 9,776,375 | 100.0% | 4,467 | 100.0% |
| By Plan Type Local Coordinated Care Plans (CCPs - HMOs and PPOs) | 510 | 83.3% | 7,184,148 | 73.5% | 3,270 | 73.2% |
| By Plan Type Private Fee For Service Plans (PFFS) | 79 | 12.9% | 2,290,955 | 23.4% | 1,000 | 22.4% |
| By Plan Type; Regional Coordinated Care Plans (CCPs - PPOs only) | 14 | 2.3% | 297,688 | 3.0% | 172 | 3.9% |
| By Plan Type Medicare Medical Savings Account Plans (MSAs) | 9 | 1.5% | 3,584 | 0.04% | 25 | 0.6% |
| By Part D Status MA-PD (1) | 594 | 97.1% | 8,314,660 | 85.0% | 3,294 | 73.7% |
| By Part D Status MA Only | 18 | 2.9% | 1,461,715 | 15.0% | 1,173 | 26.3% |
| By Special Needs Plan Status (2) Special Needs Plan (SNP) Subtotal | 443 | 72.4% | 1,267,025 | 13.0% | 770 | 17.2% |
| By Special Needs Plan Status Dual-Eligible SNPs | 270 | 44.1% | 889,809 | 9.1% | 440 | 9.9% |
| By Special Needs Plan Status Chronic or Disabling Condition SNPs | 107 | 17.5% | 245,748 | 2.5% | 241 | 5.4% |
| By Special Needs Plan Status Institutional SNPs | 66 | 10.8% | 131,468 | 1.3% | 89 | 2.0% |
| By Special Needs Plan Status Non-SNP Subtotal | 169 | 27.6% | 8,509,350 | 87.0% | 3,697 | 82.8% |
| By Group Status (3) Employer Group Only Subtotal | 348 | 56.9% | 1,697,848 | 17.4% | 1,086 | 24.3% |
| By Group Status Employer / Union Only Group Waiver Plans (800 Series) | 346 | 56.5% | 1,684,651 | 17.2% | 1,084 | 24.3% |
| By Group Status Employer Direct Contract PFFS | 2 | 0.3% | 13,197 | 0.1% | 2 | 0.0% |
| By Group Status Non-Employer Group Subtotal (Individual Market) | 264 | 43.1% | 8,078,527 | 82.6% | 3,381 | 75.7% |
Overall, MA enrollment increased by 68 percent between 2005 and 2008 (3.7 million new enrollees). However, enrollment increased much more rapidly for PFFS plans than for other plan types during that time period, with PFFS plans accounting for more than half of the total increase in MA enrollees (2.0 million).[19] Similarly, rural counties experienced much more rapid growth in MA enrollment when compared to urban counties, in large part due to growth in PFFS enrollment (see Table 5).
Table 5: MA Enrollment Trends, By Plan Type and County Type, 2005 vs. 2008
| Notes: Numbers may not add to totals due to rounding. The percent change for PFFS plans is particularly high because overall enrollment in these plans increased from 79,372 in March 2005 to 2,032,587 in March 2008. | ||||||
| Source: Gold et. al., 2008 | ||||||
| Plan Type | Total | Urban | Rural | |||
| Net Increase in MA Enrollees, 2005 vs. 2008 | % Change in MA Enrollees, 2005 vs. 2008 | Net Increase in MA Enrollees, 2005 vs. 2008 | % Change in MA Enrollees, 2005 vs. 2008 | Net Increase in MA Enrollees, 2005 vs. 2008 | % Change in MA Enrollees, 2005 vs. 2008 | |
| Local Coordinated Care Plans (HMOs, PPOs) | 1.6M | 33.0% | 1.5M | 31.2% | 0.2M | 128.3% |
| Private Fee For Service Plans (PFFS) | 2.0M | 2472.2% | 1.4M | 2511.1% | 0.6M | 2296.2% |
| Regional Coordinated Care Plans (PPOs) | 0.3M | n/a | 0.2M | n/a | 0.1M | n/a |
| Medicare Medical Savings Account Plans (MSAs, excludes Demos) | 1.7K | n/a | 1.4K | n/a | 0.3K | n/a |
| Total - All Medicare Advantage Plans (excludes Cost, PACE, Demos, Pilots) | 3.7M | 68.2% | 2.8M | 54.8% | 0.9M | 367.2% |
Minorities comprise a slightly higher proportion of the MA enrollees (27 percent in 2007) when compared with the FFS population (20 percent). There is a possibility that a correlation may exist between race / ethnicity and income for MA enrollees. The MA program has a smaller share of enrollees with incomes below $10,000[20] (15 percent in 2007) when compared with the FFS program (22 percent, excluding those who have Medigap supplemental coverage) because some of these beneficiaries may have supplemental coverage through Medicaid or through the Medicare Savings Program. However, the MA program has a somewhat higher proportion of enrollees with incomes falling between $10,000 and $30,000[21] (57 percent) when compared with the traditional FFS program (46 percent).
Nearly half of the nation?s MA enrollees were concentrated in four States in 2008: California (16 percent), Florida (9 percent), New York (8 percent), and
Pennsylvania (8 percent). However, as MA plan availability has expanded over the past few years, these States now account for a smaller share of total MA enrollment (41 percent in 2008 vs. 56 percent in 2005).
MA enrollment continues to be concentrated among a relatively small number of firms, with four firms accounting for 52 percent of MA enrollment in 2008: United Healthcare / Secure Horizons (13 percent), Humana (12.8 percent), Kaiser Permanente (9.6 percent), and the various Blue Cross / Blue Shield affiliates (16 percent). However their share of the market has decreased (59 percent in 2005) as more firms have entered the program with nearly national offerings (Gold et. al., 2008).
[ Go to Contents ]
Comparing Medicare Advantage and Fee-For-Service Payments
The policies implemented under both BBA and MMA, particularly payment floors, have had a substantial impact on MA payments in comparison to FFS payments. Current MA benchmarks and payments in the floor counties are substantially higher than comparable FFS costs. For example, in 2006, MA payments in large urban and other floor counties were 17 and 28 percent higher than FFS costs on average, respectfully, while MA payments in non-floor counties were only 6 percent higher than FFS costs (see Table 6).
Table 6: FFS Expenditures vs. MA Benchmarks and Payments, By Floor Status, 2006
| Source: MedPAC, March 2007 Report to Congress | ||||
| Floor Status of Counties | 2006 Benchmark Relative to FFS Expenditures | 2006 Payments for MA Enrollees Relative to FFS Expenditures | July 2006 MA Enrollment (thousands) | Percent of Total |
| Nonfloor | 111% | 106% | 3,394 | 49% |
| Large Urban Floor | 121% | 117% | 2,683 | 39% |
| Other Floor | 134% | 128% | 800 | 12% |
| National Average - All MA Plans With Bids (including Puerto Rico) | 116% | 112% | 6,877 | 100% |
The payment floors? impact on MA payments has been increasing because much of the recent growth in MA enrollment has been disproportionately concentrated in floor counties. For example, while urban and rural floor counties accounted for 30 percent of all M+C enrollees in 2005, these counties accounted for 42 percent of all MA enrollees in 2008 (see Table 7).
Table 7: MA Enrollment Trends, By M+C Program County Payment Type, 2005-2008
| Note: This table holds the 2004 M+C program county payment type constant, and compares 2005 M+C enrollment vs. 2008 MA enrollment in these counties. | ||||
| Source: Gold et. al., 2008 | ||||
| 2004 M+C Program County Payment Type | 2005% of Total Medicare Beneficiaries | 2005% of Total M+C Enrollees | 2008% of Total MA Enrollees | 2005-2008% Change in Enrollment |
| Rural Floor | 17.6% | 3.9% | 10.6% | 350.7% |
| Urban Floor | 28.3% | 26.9% | 31.8% | 98.6% |
| 100% FFS | 37.6% | 40.7% | 36.3% | 50.2% |
| Blend | 4.1% | 7.2% | 5.3% | 23.5% |
| Minimum Increase | 12.4% | 21.2% | 16.0% | 27.0% |
| Total - All Counties | 100.0% | 100.0% | 100.0% | 68.2% |
It is also important to note that the proportion of MA enrollees in floor counties varies by plan type. For example, in 2008, rural and floor counties accounted for 69 percent of PFFS plan enrollment, but only accounted for 29 percent of Local HMO plan enrollment (see Table 8).
Table 8: MA Enrollment, By Plan Type and Floor Status, 2008
| Source: Gold et. al., 2008 | ||||
| 2008 MA Program County Payment Type | Total | Local HMOs | Local PPOs | PFFS |
| Rural Floor | 10.0% | 3.3% | 8.7% | 28.2% |
| Urban Floor | 30.8% | 26.1% | 42.9% | 41.1% |
| All Others | 59.2% | 70.6% | 48.4% | 30.7% |
| Total - All Counties | 100.0% | 100.0% | 100.0% | 100.0% |
The net results of the benchmarks exceeding FFS costs and the enrollment trends is that payments to MA plans are considerably greater than would be the costs for comparable patients under the traditional program. For example, in 2008, the MA benchmarks were 18 percent higher than FFS expenditures, on average. Additionally, while plans? bids were only 1 percent higher than FFS expenditures on average, because plans received 75 percent of the difference between their bids and the benchmarks, actual MA program payments were 13 percent higher than FFS expenditures, on average (see Table 9).[22]
Table 9: MA Benchmarks, Bids and Payments vs. FFS Expenditures, By Plan Type, 2008
| Sources: MedPAC, March 2008 Report to Congress; Zarabozo and Harrison, 2008 | ||||
| Description | MA BENCHMARKS as a % of FFS Expenditures (includes local and regional benchmarks) | MA BIDS as a % of FFS Expenditures(represents bids for Medicare Part A and Part B benefits) | MA Program PAYMENTS as a % of FFS Expenditures (bids plus rebates representing 75% of the difference between bids and benchmarks) | MA Program REBATES as a % of FFS Expenditures(represents 75% of the difference between bids and benchmarks for plans bidding below the benchmark) |
| All MA Plans with Bids(including Puerto Rico) | 118% | 101% | 113% | 13% |
| HMOs | 117% | 99% | 112% | 14% |
| Local PPOs | 122% | 108% | 119% | 11% |
| Regional PPOs | 115% | 103% | 112% | 9% |
| PFFS | 120% | 108% | 117% | 9% |
Meanwhile, MA payments to PFFS plans and Local PPOs, which tend to have more enrollees concentrated in the urban and rural floor counties, were 17 percent and 19 percent higher than comparable FFS expenditures in 2008. On the other hand, MA payments to local HMOs and Regional PPOs are 12 percent higher than FFS costs, on average during that year.
The impact of these higher payments on total Medicare spending is significant. The Congressional Budget Office (CBO) has estimated that MA program expenditures will total $91 billion for FY 2008.[23] This includes $70 billion for Local HMOs and PPOs (77 percent), $19 billion for PFFS plans (21 percent), and $2 billion for Regional PPOs (2 percent). CBO has estimated that setting the MA benchmark in each county to be equal to local per capita FFS spending would have decreased Medicare outlays for the MA program by $8.1 billion in FY 2008. Moreover, CBO has estimated that this policy would decrease spending by $64.8 billion over 5 years (FY 2008 to FY 2012), and by $159.8 billion over the 10 years including FY 2008 to FY 2017 (CBO, 2007b).
Impact on Plan Profitability
As part of their bid submissions, MA plans are currently required to submit self-reported information to CMS relating to their estimated medical and administrative costs and estimated profits, as well as actual expenditure data for the most recent full calendar year. A recent GAO study found that in 2006, there was a significant difference between MA plans? self-reported actual and projected profit margins (6.6 percent vs. 4.1 percent of total revenues, respectively), resulting in $1.3 billion more in plan profits than had been projected (GAO, 2008).[24]
[ Go to Contents ]
Evaluating MA Payment and Participation: Overarching Policy Issues
The current MA program has grown rapidly in recent years, but at a significant cost to the overall Medicare program. Thus, evaluating MA and considering payment changes has become an important and controversial policy issue. Views on the specific issues related to the current MA structure for paying plans, and options for modifying it, are often consistent with competing visions for the Medicare program. Indeed, the current debate over MA payment takes place and is perhaps best understood within the context of a larger historical debate over the role of private plans in the Medicare program. In the following sections we describe these issues.
Medicare is one of the largest and most popular social programs in the United States. It has provided a stable source of health insurance coverage for aged and disabled individuals for over forty years, and now covers 45 million beneficiaries (as of November 2008). Along with Social Security, Medicare?s coverage assures some financial security for the elderly and disabled. In addition, Medicare has also provided public health benefits by arguably supporting health care infrastructure and innovation through its timely and consistent payments to health care providers; and helping to assure an adequate supply of physicians through its support of medical education programs.
Nonetheless, the fiscal challenges Medicare faces in the 21st century are formidable. The rapidly rising costs of providing health care to the Medicare population will result in difficult choices for policymakers in terms of assuring the program?s long run sustainability. Under current law projections, outlays from the Part A trust fund began to exceed income in 2008 and the fund will be exhausted in 2019. Moreover, under a provision of the MMA, prescribed policy responses are ?triggered? when general tax revenue funding is projected to exceed 45 percent of Medicare?s total spending. According to the latest projections, the 45 percent threshold will be breached in 2014 and the percent of spending accounted for by general revenues will grow steadily afterwards ? meaning that the size of the spending reductions needed to address the ?trigger? will grow rapidly. Moreover, the program?s future impact on the Federal budget and the aggregate economy is significant. Medicare overall is projected to grow to nearly 6 percent of the gross Domestic Product (GDP) by 2030 (2008 Medicare Trustees Report).
In addition to the fiscal issues, the quality of care for Medicare beneficiaries, as in the health system as a whole is considered disappointing (Gold, 2008). Thus, the value of health care provided to beneficiaries ? the outcomes per dollar spent ? is considered to be suboptimal. Another indicator of these problems is the considerable variation in Medicare spending per beneficiary among geographic areas. These variations cannot be explained by local price differences or beneficiary characteristics, and higher spending areas are not associated with better quality of care (CBO, 2007a).
[ Go to Contents ]
Competing Views on the Role of Private Plans in Medicare
These significant policy challenges set the stage for new rounds of the longstanding debate over the appropriate approach to the future of Medicare. On one hand, there is support among many policy makers for the view that the best option for improving the value of care and financial sustainability of Medicare is a dynamic marketplace of competing private health plans. These analysts see the problems described above as a direct result of the incentives inherent in Medicare?s fee for service payment systems and rules. They believe that Medicare?s size, decision making / policy implementation structure, and politics render the traditional program incapable of meeting the challenges of a rapidly changing health care system on behalf of beneficiaries and taxpayers.
The opposing view is that while private plans have a potentially important role in Medicare for some beneficiaries, a thriving traditional program will remain the core option for assuring access to health care for beneficiaries. Proponents of this view believe that because business practices among private plans vary in response to market conditions, and these plans potentially move in and out of markets rapidly, they cannot provide a steady and secure source of coverage for most beneficiaries. They also believe that the multiple and frequent choices that would be consistent with a dynamic marketplace can be problematic for many beneficiaries. Moreover, they believe that the traditional program can best address cost and quality challenges by using use its market power and administrative structure to implement successful value based purchasing policies in the near future.
These competing visions of Medicare are based on differing ideologies concerning social and economic policies. Those more favorable in general to policies that emphasize private sector approaches over government interventions are more likely to support a Medicare program in which a significant share of beneficiaries are enrolled in private health plans. They would tend to put more weight on arguments supporting higher payments for these plans. Others believe that private markets have certain limitations for achieving social objectives and that government should assume a more active and significant role in policy implementation. They would tend to see traditional Medicare as the core program for providing coverage to a majority of beneficiaries, and see higher payments to MA plans as wasteful and a potential threat to the solvency and viability of the program. For example, they might argue that as more beneficiaries are encouraged to leave the traditional Medicare program in order to obtain the additional benefits that are available through MA plans, this would result in a de facto privatization of the current Medicare program without Congressional action having been taken.
[ Go to Contents ]
Limitations in Ability to Assess Policy Impacts
In addition to the role these differing values play in formulating the arguments concerning the role of private plans in Medicare, the debate is also difficult to evaluate for other reasons. Data and experience for estimating the potential impact of policies consistent with either view are incomplete. For this reason, it is impossible to accurately project how increasing plan participation and enrollment would eventually impact on Medicare spending ? whether under the current administered benchmark system or a fully competitive bidding system. Likewise, it is impossible to accurately assess the potential impact of new value-based purchasing policies that might be implemented under the traditional program.
Moreover, supporters of these positions tend to assess potential success for their policies under more idealized conditions than are likely to exist in the health care marketplace. Supporters of the private market approaches see health plans being driven to improve care and introduce efficiencies in order to compete for beneficiary enrollment based on price and quality. They eventually see the current benchmark system being replaced by one in which Medicare?s premium contribution is based on the outcomes of the bidding process. Such a system, as in any competitive market, means increased uncertainty about the chances for reward and the risk of financial loss for participants. Previous experience with Medicare?s competitive pricing demonstrations, which were opposed by the insurance industry, suggests that health plans are reluctant to participate under such pricing uncertainty (Berenson and Dowd, 2008). If this is the case, the goals of increasing plan participation on one hand, and realizing vigorous competition among them on the other, may be contradictory. However, while supporters of this approach tend see a minimal role for government, previous experience also suggests that ?managing? competition, particularly given the characteristics of the Medicare population, requires a considerable amount of regulation and oversight.[25]
Similarly, proponents of maintaining and strengthening the traditional program as the core source of coverage for beneficiaries see a variety of value-based purchasing (VBP) policies that can be implemented to slow spending growth and improve quality. These policies would include modifying payment systems to financially reward performance and paying for episodes of care rather than individual services. Supporters of this approach may underestimate the obstacles to implementing such polices in the near future, however. Past experience suggests that implementation of major changes in payment systems require years of research and policy development. Moreover, changes that will reduce payments to certain providers, and potentially redistribute payments among providers and geographic areas, will be politically controversial and may require compromises that somewhat reduce the desired incentives associated with these polices. Finally, past experience with new systems suggests that changes in providers? behavior tend to offset some of the anticipated impacts of the new polices, particularly if they are spending reductions, requiring years of vigilant policymaking to make adjustments that align incentives with desired outcomes.[26]
It is within the context of the competing values, visions and empirical uncertainty described above that we analyze the specific policy issues options for change in the following sections.
[ Go to Contents ]
Specific Issues for Evaluating the Current MA Payment Structure
Currently, the statutory method for setting MA payment benchmarks results in plan payments that are considerably in excess of the costs of comparable beneficiaries in the traditional Medicare program. The immediate policy debate centers on whether MA rates should remain at these levels, or whether a range of options should be considered that would reduce these rates for some or all participating health plans. There are three general questions that might be considered in evaluating these issues and options:
- What is the role and value of choices in Medicare?
- Under what circumstances, if any, should Medicare pay more for its beneficiaries to enroll in private plans than would be their cost in the traditional program?
- Should the administered MA benchmarks be replaced by benchmarks determined through a competitive bidding process?
Table 10 summarizes basic views on MA payments according to the competing visions for the Medicare program, followed by a more detailed description of specific issues.
Table 10: Competing Views on MA Payments
| Vision for the Future of Medicare | Related Policy Views on Transforming the Delivery System | Implications for Payment and Choices | |
| Analysts Emphasizing the Role of Traditional Medicare | Traditional Medicare will remain the core program for providing beneficiary coverage, MA available as a choice to meet some beneficiaries needs and preferences | Address long run cost and quality issues through aggressive VBP policies in the FFS program | Choices can be good for beneficiaries and the program, but we should not pay more than FFS for them |
| Analysts Emphasizing the Use of Market-Based Approaches | Competing private MA plans represent the future of Medicare; traditional program diminishes as a source of coverage for beneficiaries | Encourage greater competition through expanded choices and eventual implementation of competitive bidding to determine premium contributions | Choices drive the marketplace, paying more to encourage plan participation is acceptable in the short run because competition will reduce spending in the long run |
| Analysts Seeing a Role for Both Traditional Medicare and Private Plans | Both MA and the traditional program have important roles in the future of Medicare | Potentially pursue both of the above strategies | There may be select cases in which we would pay more for private plans ? e.g. high performance, innovations in care, broad geographic coverage |
[ Go to Contents ]
The Role and Value of Choices in Medicare
Often, the debate over the current MA payment structure is framed around maintaining choices for beneficiaries. Indeed, one analysis of the issue stated that:
?Individual freedom, including personal choice of different health plans and benefit options, is not negotiable? (Heritage Foundation, 2008).
In this view, choices are seen as the desirable outcome of MA payment policy. An alternative view is that choices are a means to achieving desirable outcomes rather than an end product of policy. For example, maintaining choices might have the outcome of allowing selected beneficiaries to choose coverage that better meets their individual preferences and health needs than could the traditional program. Additionally, there may be positive ?spillover effects? for the FFS program if MA plans? managed care approaches lead to modifications in provider behavior (Berenson and Dowd, 2008). Currently, the desired outcome of expanding choices would seem to be establishing a sufficient number of plans in the market, and increasing beneficiary enrollment, as a platform for vigorous competition that might eventually reduce program spending and improve value.
In either case, the MA payment policy debate might be better assessed in terms of overall value to the program, rather than simply on its impact on choices. That is, what is the overall cost of expanding and maintaining choices as opposed to the current and future benefits that might be derived from these choices (particularly with regard to reducing growth in spending)?
[ Go to Contents ]
Should the Medicare Program Pay More for Enrollment in Private Plans Than Would Be the Cost for Comparable Beneficiaries in the Traditional Program?
The key policy question, and one subject to considerable controversy, is whether the current differential in payments between MA and the traditional program should be allowed to continue or be eliminated over time. The debate is often put in terms of whether there should be a ?level playing field? or ?financial neutrality? between MA and the traditional program. Often missed in the debate is that there are really two questions to consider for policy: 1) should payments be higher in aggregate to MA plans than for comparable beneficiaries in the traditional program and; 2) should payments to MA plans be higher than in the traditional program in some market areas, even if budget neutral in aggregate?
Payment in Aggregate
Support for maintaining the higher aggregate MA payments relies on three main arguments: establishing a platform for beneficial competition in the future; the provision of benefits to MA beneficiaries above and beyond those available in the traditional program; and the opportunity for low income beneficiaries who do not qualify for Medicaid to access such additional benefits. The first argument is consistent with a vision of Medicare in which a marketplace of numerous competing health plans attracts a growing majority of beneficiaries. Since there has been past volatility in the Medicare market, and frequent statutory changes in payment policy, some believe that there is a need to establish a stable environment for plans in which there are financial incentives and ability to offer benefit packages attractive to beneficiaries. This view therefore, supports higher payment as an investment in providing a Medicare policy framework, or platform, that both allows health plans of different types to establish a foothold in the Medicare marketplace, and provides beneficiaries with experience in making informed choices among these plan options. The potential return on this investment is future reductions in Medicare spending growth and improved quality of care derived from a competitive marketplace, including one in which administered benchmarks might be replaced by those established through the bidding process.
It is also argued that the additional payments to MA plans should not be considered as overpayments because they result in beneficiaries receiving benefits that exceed those available in the traditional program. If plans? bids are less than the benchmark, they must provide additional benefits or reduced cost sharing equivalent to 75 percent of the difference between the bid and the benchmark amount. It has been estimated that the value of benefits over and above those provided by the traditional program were $55.92 per month in private fee for service plans and $71.22 in other MA plans (Merlis, 2008). To the extent that MA benchmarks were reduced, or other payment reductions were implemented, these additional benefits could be partly or fully eliminated.
As described above, low income beneficiaries who do not qualify for Medicaid (e.g., those with incomes falling between $10,000 and $30,000) comprise a somewhat higher proportion of the MA enrollment than for the traditional program. Proponents of the current MA payment structure also argue that such cuts would disproportionately affect low income and minority beneficiaries. They argue that MA plans provide an important source of supplemental coverage for these beneficiaries who might not be able to afford the extra benefits through the purchase of Medigap policies.
Opposing these arguments is the view that at least in aggregate, private plan participation in Medicare should only occur to the extent that these plans can operate at the same or lower cost than the traditional program. Especially given the unfavorable projections for Medicare?s solvency, supporters of this view believe it is fiscally unwise to be increasing spending by a significant amount to expand or maintain the MA program. Proponents of this view believe the higher payments to plans undermine the original rationale for private plan participation ? greater efficiency and cost savings for the program. They believe that the higher payments allow plans to compete for beneficiary enrollments based on added benefits without the need to become more efficient, for example by exploring innovations in care that would reduce costs and increase quality. Indeed, one analysis of the issue stated that:
?neither public nor private plans need be artificially ?propped up? by special subsidies. In a market characterized by a level playing field, the best judge of the relative advantages of public versus private plans is the beneficiary? (Berenson and Dowd, 2008).
In addition, there is doubt about whether the current increase in spending represents a prudent investment in future cost savings that might be generated by a competitive marketplace. In the past, plans have resisted competitive bidding and have rapidly withdrawn from the Medicare markets when the program?s payment to them was deemed unfavorable. Thus, the additional spending borne by both the taxpayers and those beneficiaries remaining in the traditional program (through higher Part B premiums) is seen as wasteful and inequitable.
In addition, the value of additional benefits provided to beneficiaries through the MA plans has been questioned. These added benefits have not been put to a full market test of their value because they are subsidized by benchmarks that may be artificially high. In addition, the actuarial value calculated for these benefits, ($55.92 per month for PFFS plans and $71.22 for other MA plans in 2006) seems to fall short of the additional payments to plans of about $90.00 per month in 2006. The difference between the additional benefits and payments is much larger for the PFFS plans ? CBO has estimated that these plans are paid 19 percent more than would be the cost of beneficiaries in the traditional program but provide added benefits that are 10 percent greater than in the traditional program (CBO, 2008a). Besides the questions concerning the value of these benefits, issues of equity have been raised with regard to the increasing program spending to provide added benefits only for beneficiaries who choose to enroll in an MA plan. Since the additional costs raise the Part B premium for all beneficiaries, those remaining in the traditional program must finance part of the additional benefits provided to those in MA plans. Those who consider this cross subsidization to be inequitable argue that if the policy objective is to increase spending for enhanced Medicare benefits, these benefits should be provided to those choosing the traditional program as well.
Finally, it is argued that while the objective of making additional benefits available to low income beneficiaries is laudable, higher payments to MA plans is a poorly targeted and wasteful method of achieving this end (Park and Trisi, 2008).[27] That is, direct subsidies to beneficiaries who meet certain income criteria might be a more efficient way of achieving this policy objective.
[ Go to Contents ]
Should Payments to MA Plans Equal the Costs of Providing Benefits in the Traditional Program for All Local Markets and Types of Plans?
Whether total payments to MA plans are budget neutral relative to comparable beneficiaries in the traditional program or not, there are separate policy issues related to whether there should be payment equivalence in each local market. MedPAC has recommended financial neutrality between payments in the traditional program and payments to private plans ? sometimes referred to as a level playing field (MedPAC 2007, 2008a). In this approach, benchmarks would be set equal to fee for service costs in each market. Thus, financial neutrality occurs within each local market and payments in aggregate would either be neutral to beneficiaries? choices between the traditional program and MA, or produce a savings for the program as a whole (to the extent plans bid below the new benchmarks). MedPAC believes that while fee for service costs do not necessarily reflect efficient care in each market, at minimum MA plans should face the financial pressure to reduce the costs of care below those of the traditional program.
An opposing view is that the level playing field does not mean financial neutrality at the local level for several reasons. They believe that the objective of MA payment policy should be to provide incentives for plans to become as efficient as possible given local market conditions. That is, plans should have the incentive to base their bids on the lowest market-based costs achievable while being consistent with high quality care. Proponents of this view believe that Medicare?s fee for service costs represent an inadequate standard for reflecting local market conditions and for achieving this objective. Due to a combination of Medicare?s monopsony power to set prices on one hand, but limitations for encouraging efficient care on the other, local fee for services costs may understate the costs of efficient care in some markets and overestimate the costs of efficient care in others (Berenson and Dowd, 2008). The significant variation in costs among geographic areas provides some support for this argument while a CBO study demonstrated that plans? actual costs could range from 40 percent below to 40 percent above local per capita fee for service costs.
Therefore, in contrast to leveling the playing field, financial neutrality at the local level may advantage MA plans in some areas relative to the traditional program and disadvantage them in other areas. A number of analyses have demonstrated that the prices private plans must pay to physicians and hospitals are much higher relative to Medicare?s fee schedule prices in rural and small metropolitan areas than in larger urban areas (Berenson, 2008). Thus, MA plans in the rural and smaller urban areas begin with a financial disadvantage relative to the traditional program. Moreover, many plans have a more limited ability to control other key components of costs such as service volume and intensity, which reflect local practice patterns and administrative overhead. As a result of these factors, costs of providing Part A and B benefits to Medicare beneficiaries vary among geographic areas differently than do costs of the traditional program. An analysis by CBO estimates that plans in areas with the highest costs for the traditional program bid on average 10 percent below these costs, while plans? bids in areas with relatively low spending in the traditional program were, on average, 21 percent higher than the traditional program costs (CBO, 2006).
For these reasons, it can be argued that even if the MA program is financially neutral in aggregate, benchmarks that differ from local fee for service costs should be allowed so that payments would more accurately reflect the true cost of care in local markets. In particular, benchmarks and payments to plans would be higher than the costs of comparable beneficiaries in the traditional program in some areas, and lower in others. It has been suggested that one way of implementing this approach would be to calculate benchmarks as a blend of national average and local fee for service costs in each area, with the blend percentages based on the variation in private health plan costs relative to the variation in local costs for traditional Medicare (Berenson, 2008).
Even if such a policy was implemented to be budget neutral in aggregate, and supported analytically based on cost differences, the basic policy question of whether the Medicare program should ever pay more for beneficiaries in private plans than it would cost for their participation in the traditional program would still need to be addressed. Consistent with the longstanding debate described above, one argument would be that the program should not pay more, even on a local level. Based on this line of thinking, if the traditional program can achieve lower costs than is possible for private plans in some markets, these plans should not receive assistance in competing for its beneficiaries. The opposing argument would be that paying more in some areas is needed to provide choices and establish the platform for competition in the future. In the following section, we discuss a potential compromise view between these two positions.
[ Go to Contents ]
Should There Be Pay for Performance in Medicare Advantage?
A potential middle ground between the competing policy positions may be the argument that Medicare should pay more for beneficiaries? participation in private plans, but only when those plans can provide care that produces value not obtainable in the traditional program. In this pay for performance (P4P) framework, plans would receive additional payments when they demonstrate that particular programs such as care coordination, disease management or other delivery innovations that cost more to operate, but provide enhanced outcomes (rather than increased benefits or reduced cost sharing) for beneficiaries.[28] Thus, payment decisions would be based on the relative value of private plans and the traditional program, as opposed to only their relative cost.
The rationale for this approach is that the traditional program has statutory, regulatory, and political limitations for implementing a variety of care management tools. Moreover, these tools may be technically more difficult to implement and operate at a national level than is the case for individual health plans at the local level. Many believe that private coordinated care plans are in a position to implement such programs and better tailor care to individual beneficiaries needs. They also believe, however, that the financial incentives have not existed to encourage MA plans to take advantage of these opportunities. The generous payments relative to the traditional program have allowed plans to compete for beneficiaries in terms of benefit enhancement and cost sharing reductions alone. Moreover, beneficiaries that might be attracted to specific care management services may be more costly to treat and thus, plans may be reluctant to operate such programs. Assuming that current risk adjustment methods adequately account for these cost differences on average, providing incentives for plans to implement care innovations may still require additional payment in order to cover their additional costs.
There may be opposition to implementing pay for performance as the only method for plans to receive payments that are higher than the costs of the traditional program. Some believe that to realize the benefits of competition, the Medicare market must contain a variety of plans to ensure sufficient choices for beneficiaries. These choices would include plans that are not necessarily structured to implement coordinated care innovations, such as PPOs and the rapidly growing PFFS plans.
There may also be opposition to providing subsidies to MA plans for providing care coordination services that they theoretically should already be providing as part of the traditional managed care service delivery model. However, it could also be argued that the P4P initiatives in the traditional FFS program would also be rewarding providers for care coordination services and quality outcomes that they should already be providing to beneficiaries, and that it would therefore be appropriate to make P4P incentives available to MA plans in the interest of providing a level playing field.
Additionally, some might argue that there is currently a lack of sufficient health outcomes measures (as opposed to process and satisfaction measures that are captured by HEDIS and CAHPS), and that this would be an important limiting factor in the ability to accurately measure and reward plan performance. They might also note that recent studies have found that traditional disease management programs through third party vendors do not hold down spending. Thus, they might argue that while there are reasons to believe that these types of programs can improve beneficiaries? health while reducing costs, there is not definitive evidence that they will lead to improved performance.
[ Go to Contents ]
Should MA Benchmarks Be Determined by a Competitive Bidding Process?
Another view of the MA payment debate casts the MA payment problem as a short-term one, eventually to be resolved by implementing a competitive bidding process to determine benchmarks. In this view, achieving long-run efficiency (and savings) for the Medicare program means determining the ?right? prices (benchmarks) over time. These are benchmarks that provide the appropriate incentives for health plans to: 1) participate in the Medicare market and 2) develop innovations for delivering high quality care at the lowest possible cost. Many believe that an administered pricing system cannot provide these appropriate prices on a continuous basis. Rather, such prices can only be determined by the ongoing operation of the marketplace, enhanced by a fully competitive bidding process.
Although the current MA program does determine payments to plans based on a bidding process, it involves bidding relative to a known, administered benchmark, rather than a process in which plans would be bidding against each other with an unknown benchmark that is later determined as an outcome of the process.[29] The analogy has been made that the former process mostly uses ?carrots? to affect plan performance, while the latter would use both ?carrots? and ?sticks,? since plans whose bids exceeded the bidding-based benchmark would be at a competitive disadvantage (Nichols, 2000). Particularly when administered benchmarks are generous, as many believe is the current situation; plans have the incentive to bid just low enough so that the rebate (75 percent of the difference between the bid and the benchmark) allows them to provide additional benefits to attract beneficiaries. They do not necessarily have the incentive to enter a bid which would reflect or reveal the costs of the most efficient care possible.[30]
In contrast, in a true competitive bidding or pricing process plans would know neither what the benchmark will be, nor how potential competitors will structure their bids. Benchmarks would be based on the bid data ? for example, as a weighted average of bids, median bid or minimum bid. Therefore, plans would have strong incentives to: 1) bid the lowest possible cost they can achieve for providing high quality care; and 2) be innovative with regard to modifying the delivery of care to improve efficiency over time.[31] It is in this way that proponents of increased competition among plans believe that the MA program will slow the trajectory of Medicare spending in the future.
There are numerous issues to evaluate and resolve if policymakers were to consider moving to a fully competitive bidding process in MA. The first would be the past opposition of private plans and other stakeholders to Medicare?s competitive pricing demonstration projects. Medicare has attempted three such demonstrations in the past; all have been terminated through the political process before implementation (Dowd, 2000; Nichols, 2000; Berenson and Dowd, 2008). One reason given by plans for their opposition was that the demonstrations ?tilted the playing field? because they did not include the traditional program (Ignani, 2000). Specifically, while private plans whose bids exceeded the benchmark would need to charge additional premiums to provide the basic benefit package, beneficiaries would not face the same financial penalty for choosing the traditional program when its costs for treating them were higher than the benchmark. Thus, even the efficient plans would have limited ability to attract enrollees from the traditional program.
[ Go to Contents ]
Should Traditional Medicare Be Subject to the Competitive Bidding Process?
The potential implementation of competitive bidding in MA can be thought of in two ways. First, competitive bidding may be thought of as simply a method of determining benchmarks for the participating plans that would replace the current administered benchmarks. This approach would have the narrow objective of allowing the market processes to set efficient benchmarks, but not a broader agenda of being of vehicle of overall program reform. Second, competitive bidding might be thought of in the larger context of more fundamental Medicare reform supported by some analysts and policy makers. That is, a premium support model in which the traditional program would compete with the private plans by also entering a ?bid?.
Clearly, whether the traditional program should be subject to the competitive bidding process and under what conditions might be a key issue for policymakers. Supporters of the competitive market approach to Medicare reform believe that the traditional program should be a part of the process to create a level playing field, and because they believe enrollment in traditional Medicare will be substantially reduced by the competitive process. Those who believe that the traditional program should remain the core coverage option for beneficiaries believe that if plans are more efficient, they can offer more attractive benefits to induce enrollment, but that beneficiaries need one stable and predictable option with regard to their premiums and copayments.
In addition to these competing views, there would be several technical details to consider. For example, would the traditional program?s default bid be local fee for service costs, or would the program develop actual bids for providing services? Would the traditional program be given the authority to add benefits when their bids were less than the benchmark? Would the traditional program be given authority to use the same managed care/purchasing tools that MA plans can employ ? for example, selective contracting with providers, entering risk arrangements and developing care coordination techniques? Would the traditional Medicare program be allowed to offer an integrated product that includes medical, drug and supplemental coverage? Would the traditional program be required to include the proportion of administrative costs that it shares with other government agencies (e.g.,
Social Security, U.S. Postal Service) in its premiums? Would the traditional program be required to report the same kinds of detailed financial and quality information as MA plans? All of these questions might need to be resolved before the competitive playing field was considered as level.
Additional Considerations Regarding Competitive Bidding
In addition to determining how the traditional program should participate, policymakers might consider a variety of other issues and concerns that have been raised regarding competitive pricing (e.g., using competitive bidding to set MA plan payments). First, it is not clear that health plans will see a good business case for participating in the Medicare market under the conditions of uncertainty, and potentially lower prices, that competitive bidding would engender. One lesson learned from the failed demonstrations by some former CMS officials was that ?it?s hard to save money and get lots of Medicare beneficiaries into lots of HMOs? (Cooper and Vladeck, 2000). As discussed previously, the goals of multiple plan choices and rapidly growing MA enrollment may be incompatible with the goal of reducing spending for the Medicare program. Because the administrative costs for some private plans are much higher than for the traditional program, these plans would have to be considerably more efficient in order to simultaneously save money for the program, provide extra benefits and earn a sufficient profit. Moreover, depending on competition in different markets, the change in benchmarks from year to year might be less predictable than under the current system. It is possible that plans would not find a Medicare market that is based on competitive bidding to be a desirable one in which to participate ? overall, and/or in certain geographic areas.
In addition, if competitive bidding is to be successful at bringing value to the Medicare program, the eventual impacts on the participation of certain types of MA plans may be similar to those that would occur if administered benchmarks are reduced. One concern about proposals to reduce current benchmarks to fee for service levels is that certain types of plans such as private fee for service and local PPOs (whose enrollees are disproportionately concentrated in floor counties, where the discrepancy between current benchmarks and FFS costs is greatest) would be disadvantaged and withdraw from the market. But if competitive bidding is successful, payments to plans will grow at a slower rate than fee for service costs over time, and eventually not only eliminate the current amount by which MA payments exceed fee for services costs but reduce payments below fee for service costs as well. Potentially, only plans with the ability to develop and successfully implement innovations in the delivery of care that significantly increase efficiency will be able to compete in such a marketplace. While HMO coordinated care plans may be able to achieve these successes, it is less likely that the private fee for service plans and PPOs would be able to offer viable competition under these conditions, since they are not necessarily structured for care management and coordination (PPOs? existing networks of contracted providers, and the MIPPA requirement for most PFFS plans to develop similar networks by 2011, could potentially assist these plans in coordinating care). Thus, while these market effects attributable to competitive bidding may take place over a longer time period, and are potentially more nuanced in specific markets, they may be very much the same in terms of plan participation and enrollment as would have occurred through reductions in administered benchmarks.
[ Go to Contents ]
The General Context for Considering Policy Options
In considering potential payment policy modifications for the MA program, policymakers will face a variety of issues and competing preferences. The current program has been experiencing rapid enrollment growth, with more than 20 percent of all beneficiaries in MA plans as of 2008. However, the costs of the program are significant. CBO has estimated that payments to MA plans are on average 13 percent greater than the costs of comparable beneficiaries in the traditional program. The impact on program expenditures is more than $150 billion over ten years. MA enrollees receive additional benefits relative to the traditional program, but the value of these benefits and the equity of their financing have been questioned. Moreover, quality of care and outcomes has been found to be similar between MA plans and the traditional program, raising further questions about the value of the additional spending. On the other hand, it has been argued that the added costs are an investment in establishing a platform for vigorous competition that will eventually reduce Medicare cost growth.
[ Go to Contents ]
Short-Term Versus Long-Term Approaches
An MA program that offered meaningful choices to beneficiaries, provided care innovations that improved quality, and resulted in lower aggregate costs might make an important contribution to the future health of Medicare. For many reasons, a competitive bidding model for determining the annual MA benchmarks would likely be the preferable long-run policy option for achieving these objectives. A well-functioning bidding process could be essential for establishing market-based prices that reflected local market conditions, encouraged plan participation and simultaneously provided incentives for high-value health care.
Nonetheless, there may be policy rationales for transitioning to a full competitive bidding model over a longer time period. Competitive pricing has been politically controversial for many years, and it is likely that policy compromises will be difficult to achieve. As discussed above, there are numerous and difficult policy decisions that would need to be made. Moreover, a provision of the MMA has established a Comparative Cost Adjustment (CCA) demonstration to begin in 2010. The demonstration would test a competitive pricing model, including the traditional program, in a limited number of localities. It is possible that policymakers would want to wait until the results of these demonstrations are well evaluated before implementing competitive pricing more broadly, but this will not be until a number of years into the future.[32]
Thus, addressing MA payment issues in the foreseeable future is likely to involve considering options, potentially as short-term or transitional approaches, which would continue to rely on administered benchmarks in their current or modified forms. These policy choices might include maintaining current policy to assure continued growth in plan and beneficiary participation. Alternatively, there are a number of choices directed at modifying current payment parameters in order to achieve budget savings and address equity concerns. In addition, changes to the current payment parameters could be structured in order to better recognize local market conditions and encourage greater competition between plans in terms of efficiency and quality.
Should policy makers decide to modify how MA payments are determined, there would be several aspects of the current methodology that could be modified. The current payments are based on the established benchmarks (which no longer are well-calibrated to local FFS costs), the plan?s bid, and the specific formula for determining rebates to plans when they bid below the benchmark. Thus, payment options might include: determining benchmarks through competitive bidding; recalibrating the administered benchmarks; finding new ways to calculate the rebates to plans; or a combination of these approaches.
[ Go to Contents ]
Potential Market Impacts
Any option being considered that would reduce payments to MA plans is likely to result in a number of market impacts. In particular, plans will decide whether they can continue to offer a benefit package in a given geographic area that will remain competitive while maintaining their profit margins. Beneficiaries will respond to any changes in plan offerings as they make choices between the various plans and the traditional program. In general, it may be reasonable to expect a variety of effects in response to MA payment reductions:
- Some plans would make efforts to become more efficient in order to remain competitive under the lower rates;
- Some plans would stay in the market but reduce the value of the supplemental benefits they provide;
- Some plans would withdraw from the Medicare market;
- Some beneficiaries enrolled in MA would switch plans or return to the traditional program;
- Beneficiaries in the traditional program who might have enrolled in MA under current arrangements may choose not to make a change;
- New beneficiaries who might have chosen to enroll in MA may decide on the traditional program instead.
The net effect of these changes is likely to be a reduction in the projected rate of growth in MA enrollment, including reduced plan participation (CBO, 2007b, 2009).
[ Go to Contents ]
Approach for Estimating the Impacts of Policy Options
The impacts of the various options are estimated using a model developed from county level MA data, which were supplemented by distributions from plan level bidding and payment data. The county level data included the 2008 benchmark, per capita FFS costs, enrollment by major type of plan (including Local HMOs, Local PPOs, Regional PPOs, and PFFS plans), MA penetration and an indicator of the county?s payment status (rural floor, urban floor, blend, etc.). Based on plan level bidding and payment data, a distribution of bids and payments was developed for each major plan and county type. The model was developed to estimate impacts on payments to MA plans and beneficiary enrollment in MA.
The impacts for each option were estimated relative to CBO?s baseline for MA payment and enrollment (CBO, 2007b, 2009). Medicare expenditure impacts were estimated based on two components: the difference between the baseline spending and MA spending under each option for beneficiaries who would be projected to remain in MA under the option; plus the difference between baseline MA spending and FFS spending for beneficiaries projected to switch to the traditional program as a result of the option. It was assumed that the first year of implementation for each option would be 2011.
It should be noted that at this time, the impact model is static with regard to plans? responses. Specifically, changes in enrollment are based on the estimated relationship between MA take-up rates and MA plan payments from previous years? data. We do not assume any specific behavioral changes on the part of plans in response to these policies with regard to efficiency and bidding strategy. To the extent that plans do respond to any of the options by finding ways to reduce bids and to some degree maintain the additional benefits they currently provide, the projections may underestimate spending reductions and overestimate the reductions in enrollment that would occur. It is likely that such responses would differ among the options. For example, it is possible that the modified rebate structure under Options 3 and 3a below, or the modified bidding/benchmark process under Option 4 would provide greater incentives for plans to lower their bids than would Options 1 and 2. In the future, an attempt will be made to model more dynamic responses to the options.
Finally, the impacts of all of the options described below are estimated as if the policies would be fully implemented in 2011. Alternatively, any of these approaches could be implemented more gradually by transitioning to the new policy over a number of years. The latter approach would produce less short term savings, but allowing more time for plans and beneficiaries to make adjustments would potentially reduce any market disruptions that the specific payment reductions might induce. In practice, by the time any legislation is passed, it is likely to be too late to affect pricing for 2010. Therefore, plans and beneficiaries will have an extra year to begin transitioning even if the new policy was implemented fully in 2011.
[ Go to Contents ]
Specific Options for Modifying MA Benchmarks
In this section, in addition to the competitive bidding option proposed as part of the FY 2010 President?s Budget (HHS, 2009), we discuss four options for modifying the current mechanisms used to determine MA payments:
- Administered Benchmark Option 1: Set each county benchmark at estimated per capita FFS costs;
- Administered Benchmark Option 2: Set the benchmarks at a blend of local and national FFS per capita costs;
- Administered Benchmark Option 3: Retain current benchmarks but modify the structure of rebates to plans; and
- Administered Benchmark Option 4: Calculate benchmarks as a blend of current benchmarks and the average of bids for the locality.
Several variants of each of these options could be examined by slightly changing some of the parameters ? for example, by modifying the blend percentage used for the second option. In addition, while we do not evaluate a specific pay for performance option for MA payment, any of these options could be combined with basing payment on measures of performance. Further research is needed to determine what types of services or care innovations could be implemented by MA plans to improve quality and value. Such policies might be budget neutral to a desired level of aggregate spending and redistribute some portion of payments among MA plans based on their relative performance. Alternatively, pay for performance might be used to increase aggregate MA payments based on performance or value that exceeds that being provided in the traditional program.
In evaluating these options, we discuss potential advantages and disadvantages that are unique to each of them. It should be noted that all of the options are projected to result in substantial reductions in payments to MA plans and resulting reductions in beneficiary enrollment. How potentially harmful or beneficial these reductions are perceived to be for the Medicare program is likely to depend on the policy views discussed earlier in the paper. For those who believe in private market competition as the future of Medicare, these reductions would be seen as a significant obstacle to the long run sustainability of the program. For those who believe in some measure of financial neutrality between MA and the traditional program, these reductions would be seen as a necessary adjustment from participation levels that occurred due to the incentives created by inappropriately high MA payment levels.
[ Go to Contents ]
President?s Budget Option: Competitive Bidding
Under this option, the current administered benchmarks would be eliminated and replaced with an enrollment-weighted average of the bids in each year. All plans would receive this benchmark amount. Thus, plans whose bids were below the benchmark would receive 100 percent of the difference between the bid and the benchmark (rather than the current 75 percent) while plans whose bids exceeded the benchmark would need to charge additional premiums to beneficiaries. Competitive bidding under this option would apply only to MA plans and not include the traditional Medicare program.
The rationale for this option is as discussed above. Because plans would be bidding against each other, rather than against a known benchmark, they would have a greater incentive to structure bids that reflected the lowest costs possible for providing high quality care in a given area. The benchmark would then reflect the local price for providing efficient care, as determined by a market mechanism rather than based on an administered amount. The market-based mechanism would likely encourage long- run cost savings, while at the same time being more sensitive to local market variations than the current administered benchmarks.
The potential disadvantage of this approach is that plans would potentially be averse to the combination of the likely lower benchmarks that would occur under a competitive bidding system and the risk associated with not knowing the benchmark at the time that the bid is submitted. The result might be a reduction in participating plans in some or all markets.
Impacts
The CBO has estimated that this proposal would save $160 billion through 2019 and result in enrollment reductions of slightly more than 50 percent (for example, CBO estimates that 7 million fewer beneficiaries would be enrolled in MA plans in 2019, versus 13.9 million under current law). CBO also estimates that implementing competitive bidding with pay-for-performance bonus payments for plans that implement value-based quality improvement mechanisms would reduce the estimated savings by about $50 billion, but would also reduce the projected enrollment reductions to 20 percent or 2.6 million beneficiaries in 2019 (CBO, 2009).
[ Go to Contents ]
Administered Benchmark Option 1: Set County Benchmarks Equal to Local Per Capita FFS Costs
Under this option, each county benchmark would be recalculated to equal the most recent estimate for per capita fee for service costs adjusted to the appropriate payment year. All other payment parameters would remain the same as under current law so that plans whose bids were below the new benchmarks would be paid their bid plus 75 percent of the difference between the bid and the benchmark. Plans whose bids were above the benchmark would be paid the benchmark rate and be required to increase beneficiary premiums in the amount of the difference.
There are two related rationales for this option. The first rationale is that the Medicare program?s subsidy should be financially neutral within local markets with regard to beneficiaries? choice of coverage. That is, the program should pay no more on a risk adjusted basis for beneficiaries? participation in private plans than if they chose the traditional program. In addition to potentially being more equitable among beneficiaries, such financial neutrality would produce significant long run budget savings. The second rationale is that because the current benchmarks have been modified through legislation, they no longer accurately reflect the local FFS costs on which they were originally based, or any reasonable measure of private market costs of care. Thus, setting benchmarks at local FFS costs would better reflect the costs of providing care in local health care markets and therefore provide a better benchmark for bidding. Moreover, the reduced benchmarks would provide greater incentives for plans to compete with each other by finding ways to more efficiently provide high quality care.
There are also likely to be perceived disadvantages to this approach. For the reasons described above, private market costs may vary from locality to locality in a different manner than do local FFS costs. They may be higher than FFS costs in some markets and lower in others. Thus, plans in the localities for which FFS costs underestimate private market costs would be disadvantaged in competing with the traditional program for enrollment. Conversely, plans in localities for which FFS costs are high relative to private market costs could compete well with the traditional program.
Impacts
If fully implemented for 2011, this option would produce savings of approximately 12 percent for the Medicare program in each year (which is somewhat larger than the estimated savings for the competitive bidding option discussed above). Based on these simulations, the payment reductions would result in MA enrollment declining by approximately 50 percent in each year.
The projected payment reductions would be larger for PFFS plans and Local PPOs, slightly more than 14 percent for the former and nearly 15 percent for the latter. In addition, the reductions are projected to be about 15 percent for urban and rural floor counties. Corresponding to these payment reductions, projected enrollment reductions for these types of plans and counties would be proportionally larger than the aggregate impact.
[ Go to Contents ]
Administered Benchmark Option 2: Set MA Benchmarks at a Blend of Local and National Average FFS Costs
Option 2 would replace the existing MA benchmarks with a benchmark calculated as a blend of local and national average per capita FFS costs. For purposes of this paper, we analyze a blend calculated as 50 percent local FFS cost and 50 percent national weighted average FFS cost. In the future, we will further analyze the relationships between local FFS costs, plan bids and other measures of local cost to determine if other blend percentages might be appropriate.[33] All other payment parameters for this option would remain the same as under current law.
One rationale for this approach is similar to that of Option 1 ? the current benchmarks do not accurately reflect the costs of providing care in local areas. Unlike Option 1, however, this option also would be based on the rationale that local FFS costs are not accurate indicators of the cost of providing care in these markets either. The blend represents a standard partly based on costs that reasonably do not vary significantly among localities (e.g., administrative costs) and those that may not vary significantly between Medicare FFS and private markets within a locality (e.g., practice patterns) on one hand; and partly based on costs that do vary among areas (e.g., hospital and physician prices) on the other. Operationally, national average FFS cost becomes a proxy for an efficient level of costs that do not vary substantially and county level FFS costs reflect local variations that should be recognized in the benchmarks. While the blended benchmarks would be considerably lower than the current benchmarks in most localities, they would be higher than FFS costs for the below average cost counties and lower than FFS for the highest cost counties.
A potential disadvantage to this approach is that the blend may not provide a reasonable standard for the costs of efficiently providing care. The underlying theory for this approach is that the blend should reflect differences in the way private market costs of providing care vary relative to the way Medicare?s local FFS costs vary. Currently, there is not sufficient research or data to provide an understanding of the variation in local private market costs. While the MA plans? bids can be analyzed, they reflect the plans? offers relative to benchmarks which are considered to be high relative to the efficient cost of care. Therefore, these bids may not reflect the best costs that are achievable in the marketplace and it is not clear to what extent the blended benchmark is an improvement over one based only on local FFS costs.
Impacts
The spending impacts for this option are projected to be similar to those of Option 1 ? approximately 12 percent. The impact on enrollment would be somewhat smaller than for Option 1, however, because the payment reductions would be smaller for PFFS plans and in rural floor counties than under a strictly local FFS benchmark.
Indeed, PFFS plans are projected to experience a payment reduction of 11 percent relative to the aggregate impact of 12 percent for this option, compared with a reduction of over 14 percent under Option 1. Plans in rural floor counties would experience a smaller than average reduction of approximately 8 percent, while plans in urban floor counties would experience a reduction equivalent to the average. Payment reductions for plans in FFS counties would be about 10 percent, relative to a very small reduction under Option 1. This is because these counties have much higher than average FFS costs and therefore are disproportionately affected by a benchmark partly based on the national average.
[ Go to Contents ]
Administered Benchmark Option 3: Maintain Current Benchmarks but Modify the Rebate Structure
Under this option, rebates and therefore payments to plans would be determined by the relationship of the plans? bids to two benchmarks: the current county level benchmark and the county level FFS costs. Specifically, plans bidding below the current benchmark but above current FFS costs would receive a rebate equal to 25 percent of the difference between the bid and the benchmark. Plans whose bids were also below FFS costs would receive a rebate equal to 25 percent of the difference between county level FFS cost and the benchmark plus 75 percent of the difference between the bid and the county level FFS cost.
The rationale for this option is twofold: 1) maintain the current benchmarks that while high relative to FFS costs have encouraged plan participation and beneficiary enrollment; but 2) modify the rebate structure in a way that provides financial incentives that encourage plans to implement care and other innovations that reduce costs. This option may encourage a more competitive bidding process among plans than under current law since the ?kinked? rebate structure means that plans that were able to reduce their bids to below FFS costs would have a significant advantage in attracting beneficiary enrollment over plans that cannot reduce their costs as much. At the same time, plans that could not immediately bring their bids below FFS costs would not have to charge additional premiums to beneficiaries (as would be the case under Option 1) and would still receive some rebate to provide additional benefits, as long as their bid was below current benchmarks. Moreover, these plans would have the incentive to reduce their bids further below benchmarks than under the current system ? even if remaining above FFS costs ? in order to minimize any reduction in the additional benefits they could provide with the reduced rebate percentage.
A disadvantage of this approach is that that MA payment would be based on a combination of two benchmarks, although neither may reflect the cost of efficiently providing care in the local markets. To some extent, this option often shares the disadvantages discussed relative to Option 1. Plans in areas for which FFS costs underestimate the private market costs of providing care would face disadvantages in structuring bids that were less than the lower benchmark. Another disadvantage to this approach is that, at least initially, payments to MA plans would remain higher in aggregate than would occur if beneficiaries were enrolled in the traditional program. The rebate calculations could be changed immediately or over time, however, to achieve greater budget savings. For example, the rebate percentages paid for bids above FFS costs, those below FFS costs, or both could be reduced.
Impacts
The likely spending impacts of this option are smaller than for the previous options since it would allow a far greater number of plans to receive payments in excess of FFS costs. The 2011 impact would be a reduction of approximately 7.5 percent. Correspondingly, the enrollment impact would be also be smaller, a reduction in each year of about 20 percent. If the rebate percentage for bids below FFS costs were reduced from 75 percent to 50 percent, the spending impact would increase from 7.5 percent to 9.0 percent.
In general, the impacts of this option on different types of plans and localities do not differ significantly from the aggregate. The one exception is that plans in rural floor counties are projected to experience a payment reduction that would be smaller than the average ? approximately 4.5 percent.
[ Go to Contents ]
Administered Benchmark Option 3a ? Option 3 but Replace the FFS Cost Benchmark with a Blended Benchmark
This option would operate in the same manner as Option 3 except that the ?lower? benchmark would be the blend of 50 percent national average FFS costs and 50 percent local FFS costs. The rationale would be similar to those described for Option 2. It would balance the perceived disadvantages faced by plans in relatively low FFS cost areas relative to those in the high FFS cost localities.
The aggregate impact on payment would be somewhat larger than under Option 3 ? 8.7 percent rather than 7.5 percent. Most of this difference is attributable to a much larger impact for Option 3a on plans in counties that were classified as FFS, again because they are more affected by a benchmark that blends in national average costs. Conversely, plans in rural floor counties, which have the lowest average FFS costs, are less affected by options that would use a benchmark based on national average costs.
[ Go to Contents ]
Administered Benchmark Option 4 ? Set Local Benchmarks as a Blend of Current Benchmarks and the Average Bid for the Locality
Under this option, each county?s benchmark would be calculated as a blend of 50 percent based on the current benchmark and 50 percent based on an average of plans? bids from the county. The rebate determination would remain the same as under current law.
The rationale for this approach is that plans? bids in a competitive environment are the best indicators of the costs of providing efficient care in private markets. It would determine benchmarks in a manner similar to that currently used for regional MA plans and could be seen as a partial transition to an eventual system based fully on competitive bids as opposed to administered benchmarks. While implementing such system may be years off, this option would use desirable elements of both current and the potential future systems. The portion of the benchmark based on the current system would reduce some of the uncertainty plans find undesirable, the portion based on the bids would reflect costs unique to each local market. Moreover, plans would have incentives to find ways to reduce their bids since some plans whose bids were above the average bid would be at a competitive disadvantage.
A disadvantage of this approach is that plans might react negatively to bidding against an uncertain benchmark by reducing participation to a greater degree than under a known benchmark set at an equivalent amount. Under the other options, plans would not know how competitors will bid, but can compare their own bid to the known benchmark(s) to assess the attractiveness of their benefits. Under this option, plans would not know how their competitors will bid or what the final benchmark will be for comparing to their own bids.
Impacts
It is projected that spending under this option would be reduced by approximately 6 percent. Enrollment is projected to decline by somewhat less than 2 million beneficiaries relative to current law projections for each year. As with the other options, to the extent that plans responded to the new incentives provided by this option by finding ways to reduce their bids, the savings to the program could be larger and the enrollment reductions smaller.
The impacts would vary considerably by type of county. Payment would be reduced by over 9 percent in the FFS counties and by about 2 percent in the rural floor counties. The impact does not vary substantially among plan types, although the coordinated care plans would experience a slightly larger than average payment reduction under this option.
[ Go to Contents ]
Concluding Thoughts
Since the implementation of the MMA?s provisions in 2005, plan participation and enrollment in the MA program has expanded rapidly. Beneficiaries in more geographic areas now have a choice of a greater number and types of private health plans than they did prior to 2005. More than 1 in 5 beneficiaries are now enrolled in MA rather than in Medicare traditional FFS program. The expansion of MA has come at a significant cost, however. Payments to MA plans are significantly higher than would be the cost of comparable beneficiaries in the traditional Medicare program. Current estimates are that the projected enrollment in the MA program will cost approximately $150 billion more over the next ten years than if the same beneficiaries remained in the traditional program.
Whether or not the payments to MA plans should be modified to reduce or eliminate these additional costs has become a controversial policy topic. Should the Congress decide to address this issue, there would be a number of policy alternatives available that could achieve budget savings and potentially provide greater incentives for developing innovations that result in higher quality and more efficient health care being provided to beneficiaries. For a number of reasons, moving toward a system in which prices are determined by competitive bidding would be preferable. Should Congress decide to maintain an administered benchmark system for some period of time, there are a number of alternatives that reduce spending, recognize variations in local health care markets and encourage greater competition within an administered benchmark system of bidding.
[ Go to Contents ]
References
Boards Of Trustees,
Federal
Hospital Insurance And Federal Supplementary Medical Insurance Trust Funds. (2008). 2008 Annual Report Of The Boards Of Trustees Of The
Federal
Hospital Insurance And Federal Supplementary Medical Insurance Trust Funds. March 25, 2008, electronic version accessed at http://www.cms.hhs.gov/ReportsTrustFunds/downloads/tr2008.pdf.
Berenson, R.A. (2004). Medicare Disadvantaged and the Search for the ?Level Playing Field?. Health Affairs, 23 (4), w572?w585, 10.1377/hlthaff.w4.572.
Berenson, R.A. (2008). From Politics to Policy: A New Payment Approach in Medicare Advantage, Health Affairs, 27(2), 156-164.
Berenson, R.A. & Dowd, B.E. (2008). Medicare Advantage Plans At A Crossroads ? Yet Again. Health Affairs, 28(1), w29 ? w40.
Cawley, J.H. & Whitford, A.B. (2007). Improving the Design of Bidding in Medicare Advantage. Journal of Health, Politics, Policy and Law, 32(2), 317-347.
Centers for Medicare & Medicaid Services (CMS). (1996-2005). Historical Health Plan Reports, Files and Data, electronic version accessed at http://www.cms.hhs.gov/HealthPlanRepFileData/.
Centers for Medicare & Medicaid Services. (2005a) ?Medicare Program; Establishment of the Medicare Advantage Program; Final Rule.? 70 Federal Register 18 (25 January 2005), pp. 4588 - 4741.
Centers for Medicare & Medicaid Services. (2005b) ?Medicare Program; Medicare Prescription Drug Benefit; Final Rule.? 70 Federal Register 18 (25 January 2005), pp. 4194-4585.
Centers for Medicare & Medicaid Services. (2007). ?Medicare Advantage in 2007? white paper, electronic version accessed at http://www.cms.hhs.gov on May 3, 2007.
Centers for Medicare & Medicaid Services. (2008a). Announcement of Calendar Year (CY) 2009 Medicare Advantage Capitation Rates and Medicare Advantage and Part D Payment Policies, April 7, 2008, electronic version accessed at http://www.cms.hhs.gov/medicareadvtgspecratestats/downloads/announcement....
Centers for Medicare & Medicaid Services. (2008b). Medicare Advantage/Part D Contract and Enrollment Data, September 2008 and November 2008, electronic version accessed at http://www.cms.hhs.gov/MCRAdvPartDEnrolData/.
Centers for Medicare & Medicaid Services. (2008c). Medicare & You 2008, National Medicare Handbook, CMS Publication No.10050, January 2008, electronic version accessed at www.medicare.gov/Publications/Pubs/pdf/10050.pdf.
Centers for Medicare & Medicaid Services. (2008d). ?Medicare Prescription Drug Benefit?s Projected Costs Continue to Drop: Part D Attracts New Beneficiaries and Achieves High Rates of Satisfaction,? Press Release, January 31, 2008, electronic version accessed at http://www.cms.hhs.gov/center/press.asp.
Centers for Medicare & Medicaid Services. (2008e). Release of the 2009 Part D National Average Monthly Bid Amount, the Medicare Part D Base Beneficiary Premium, the Part D Regional Low-Income Premium Subsidy Amounts, and the Medicare Advantage Regional PPO Benchmarks, August 14, 2008, electronic version accessed at http://www.cms.hhs.gov/
MedicareAdvtgSpecRateStats/Downloads/PartDandMAbenchmarks2009.pdf.
Centers for Medicare & Medicaid Services. (2009a). Announcement of Calendar Year (CY) 2010 Medicare Advantage Capitation Rates and Medicare Advantage and Part D Payment Policies, April 6, 2009, electronic version accessed at http://www.cms.hhs.gov/medicareadvtgspecratestats/downloads/announcement....
Centers for Medicare & Medicaid Services. (2009b). Medicare Advantage/Part D Contract and Enrollment Data, June 2009, electronic version accessed at http://www.cms.hhs.gov/MCRAdvPartDEnrolData/.
Congressional Budget Office (CBO). (2006). Designing a Premium Support System for Medicare. December 2006.
Congressional Budget Office (CBO). (2007a). The Medicare Advantage Program: Enrollment Trends and Budgetary Effects, Statement of Peter R, Orszag before the Committee on
Finance, U.S. Senate. April 2007.
Congressional Budget Office. (2007b). The Medicare Advantage Program, Statement of Peter R, Orszag before the Committee on the Budget,
U.S. House of Representatives. June 2007.
Congressional Budget Office. (2009). Letter to Honorable Mike Crapo. May 18, 2009.
Cooper, B.S. & Vladeck, B.C. (2000). Bringing Competitive Pricing to Medicare. Health Affairs, 19(5), 49 ? 54.
Dowd, B; Coulam, R; & Feldman, R. (2000). A Tale of Four Cities: Medicare?s Experience with Competitive Pricing. Health Affairs, 19(5), 9 ? 29.
Fuchs, B. & Potetz, L. (2007). Medicare Consumer-Directed Health Plans: Medicare MSAs and HSA-Like Plans In 2007. Issue Brief.
Washington DC: Henry J. Kaiser Foundation, March 2007, electronic version accessed at http://www.kff.org/medicare/upload/7623.pdf.
Gold, M. (2007). Medicare Advantage in 2006-2007: What Congress Intended? Health Affairs, 26(4), 445-455.
Gold, M. (2008). Medicare?s Private Plans: A Report Card on Medicare Advantage. Health Affairs, 28(1), w41 ? w54.
Gold, M. & Peterson, S. (2006). Analysis of the Characteristics of Medicare Advantage Plan Participation.
Washington DC: Prepared for ASPE/HHS by Mathematica Policy Research, 2006.
Gold, M.; Taylor, E.; Fleming, C.; Phelps, D.; Cupples Hudson, M. & Loewenberg, M. (Gold et. al.) (2008). Looking at Medicare Advantage: What Has Happened Since the Launch? What Will Happen in the Future?
Washington, DC: Prepared for ASPE/HHS by Mathematica Policy Research, 2008.
Ignani, K. (2000). Putting Principles First:
A Better Way to Carry out a Demonstration. Health Affairs, 19(5), 44 -48.
Merlis, M. (2007). Medicare Advantage Payment Policy, National Health Policy Forum Background Paper. September 24, 2007.
Merlis, M. (2008). The Value of Extra Benefits Offered by Medicare Advantage Plans in 2006, Medicare Issue Brief, Henry J. Kaiser Family Foundation. January 2008.
Medicare Payment Advisory Commission (MedPAC). (2003). ?Health Insurance Choices for Medicare Beneficiaries,? Chapter 5, Report to the Congress: Medicare Payment Policy, March 2003, electronic version accessed at http://www.medpac.gov/publications/congressional_reports/Mar03_Ch5.pdf.
Medicare Payment Advisory Commission. (2004). ?Medicare+Choice Payment and Eligibility Policy,? Chapter 4, Report to the Congress: Medicare Payment Policy, March 2004.
Medicare Payment Advisory Commission. (2007). The Medicare Advantage Program and MedPAC Recommendations, Statement of Mark E. Miller Before the Committee on the Budget,
U.S. House of Representatives.
Medicare Payment Advisory Commission. (2008a). ?Update on the Medicare Advantage Program,? Chapter 3, Report to the Congress: Medicare Payment Policy, March 2008, electronic version accessed at http://www.medpac.gov/chapters/Mar08_Ch03.pdf.
Medicare Payment Advisory Commission. (2008b). ?Part D Enrollment, Benefit Offerings, and Plan Payments,? Chapter 4, Report to the Congress: Medicare Payment Policy, March 2008, electronic version accessed at http://www.medpac.gov/chapters/Mar08_Ch04.pdf.
Medicare Payment Advisory Commission. (2009a). ?The Medicare Advantage Program,? Chapter 3, Report to the Congress: Medicare Payment Policy, March 2009, electronic version accessed at http://www.medpac.gov/chapters/Mar09_Ch03.pdf.
Medicare Payment Advisory Commission. (2009b). ?Medicare Improvements for Patients and Providers Act of 2008 Medicare Advantage Payment Report,? Chapter 7, Report to the Congress: Improving Incentives in the Medicare Program, June 2009, electronic version accessed at http://www.medpac.gov/chapters/Jun09_Ch07.pdf.
Moffit, R.E. (2008). Medicare Advantage: The Case for Protecting Patient Choice, Web Memo No. 1836, Heritage Foundation.
National
Academy of Social Insurance. (2003). The Role of Private Health Plans in Medicare: Lessons from the Past, Looking to the Future, Final Report of the Study Panel on Medicare and Markets.
Nichols, L. (2000). Competitive Implications of Health Plan Pricing Rules in Medicare Reform Proposals, Testimony presented to the Senate Committee on Finance.
Nichols, L.M. & Reischauer, R.D. (2000). Who Really Wants price Competition in Medicare Managed Care? Health Affairs, 19(5), 30 ? 43.
Park, E. & Trisi, D. (2008). Improving the Medicare Savings Programs Would Help Low-Income Seniors Cope With Higher Medical Expenses. Center for Budget and Health Priorities. Electronic version accessed at http://www.cbpp.org/5-20-08health.pdf.
United States Department of Health and Human Services (HHS). (2009). Fiscal Year 2010 Budget in Brief. May 7, 2009. Electronic version accessed at http://www.hhs.gov/asrt/ob/docbudget/2010budgetinbrief.html.
U. S. Government Accountability Office (GAO). (2008). Medicare Advantage: Increased Spending Relative to Medicare Fee-for-Service May Not Always Reduce Beneficiary Out-of-Pocket Costs. GAO-08-359, February 2008, electronic version accessed at http://www.gao.gov/new.items/d08359.pdf.
U. S. House of Representatives Committees on Ways and Means, Energy and Commerce, and Education and Labor (House Committees). (2009). ?House Tri-Committee Health Reform Discussion Draft.? June 19, 2009.
Zarabozo, C.& Harrison, S. (2008). Payment Policy and the Growth of Medicare Advantage. Health Affairs, 28(1), w55 ? w67.
[ Go to Contents ]
Notes
[1] The most recent data released by the Centers for Medicare & Medicaid Services (CMS) indicate that 10.69 million of the nation?s 45.2 million beneficiaries (approximately 23.6 percent) were enrolled in MA plans as of June, 2009 (CMS, 2009b).
[2] Although only a fifth of the nation?s Medicare beneficiaries are enrolled in MA plans, all beneficiaries (including those who are enrolled in the traditional program) help to pay for the extra benefits that are being provided by MA plans through their Part B premiums.
[3] Under the M+C program, the county-level payment rates were set based on the greater of: 1) a minimum increase from the previous year?s rate (2 percent), 2) the applicable floor rate, or 3) a blend of the local rate and a national rate. The 2 percent minimum increase was designed to provide protection for private plans due to the dramatic reductions in FFS spending under the BBA (Berenson and Dowd, 2008).
[4] Local plans include health maintenance organizations (HMOs), point of service plans (POS), preferred provider organizations (PPOs), private fee-for-service (PFFS) plans, and medical savings account plans (MSA) that serve individual counties and groups of counties. MA regional plans are structured as PPOs, utilizing a network of providers, and serve all of the counties in a State or multi-State CMS-designated region.
[5] Previously, under the M+C program, Medicare?s private health plans had received a fixed administered monthly payment amount for each enrollee; however, under the MA program they were required to submit bids to provide services to Medicare beneficiaries at the local or regional level beginning with the 2006 contract year. As discussed later, it is important to note that MA program?s submission of bids against a fixed benchmark differs from a fully competitive bidding system, in which plans submit bids without knowing the benchmark in advance.
[6] Previously, PFFS plans were not required to have contracted provider networks in order to meet Medicare?s access standards; instead, they were allowed to deem that a provider had a contract with the plan if they agreed to accept Medicare fee-for-service rates as payment and met other requirements. Under the new MIPPA provision, beginning in 2011, beneficiaries in many PFFS plans that do not have provider networks are expected to either enroll in other types of MA plans, or return to the traditional FFS program.
[7] MedPAC recently released its MIPPA Medicare Advantage Payment Report in June 2009 (MedPAC, 2009b).
[8] The Medicare program also includes several types of private health plans that are not considered to be part of the Medicare Advantage program, including Cost Plans, Program of All-Inclusive Care for the Elderly (PACE), Demonstrations, and Pilots.
[9] Medicare makes an annual lump sum cash deposit into an interest-bearing medical savings account during the first month that the beneficiary?s enrollment becomes effective. This money can be used for health expenses that are not covered by the high deductible health plan (such as deductibles, copayments, and coinsurance), as well as for other qualified medical expenses, such as prescription drug, dental and vision services. Funds remaining in the medical savings account at the end of the year are the property of the enrollee, and are ?rolled over? for use during the following year. The deposits and accumulated interest in the medical savings account is tax-free. Additionally, beneficiaries and employers are not allowed to deposit additional funds into the account (Fuchs, 2007).
[10] In addition to regular MSA plans (also known as current law MSA plans), there are also MSA demonstration plans that have increased flexibility to develop benefit designs that are more similar to the consumer-directed health savings accounts (HSAs) that are available in the private sector, and are required to have service areas that comprise at least one State.
[11] Under deeming, PFFS plans are allowed to meet access requirements by offering payment rates that are not lower than those in the traditional FFS program. Providers are deemed to be part of a given PFFS plan?s network if they provide a covered service to one of the plan?s enrollees, are aware in advance that the beneficiary receiving the service is enrolled in the PFFS plan, and have reasonable access to the plan?s terms and conditions of payment.
[12] In general, beneficiaries can enroll in any MA plan during the Part D Annual Open Enrollment Period (which lasts from November 15th to December 31st each year), and they can also enroll in an MA-only plan until March 31st.
[13] For MSA plans, if the plan?s bid is below the relevant benchmark, 100 percent of the difference between the bid and the benchmark is deposited into the enrollee?s medical savings account (Fuchs, 2007).
[14] The pre-2006 historical county-level payment rates under the M+C program fell into the following categories: 1) Rural Floor, in which the M+C per capita rate was set equal to the rural floor rate; 2) Urban Floor, in which the M+C per capita rate was set equal to the urban floor rate; 3) 100 Percent of FFS, in which the M+C per capita rate was set equal to 100 percent of local per capita FFS costs; 4) Blend, in which the M+C per capita rate was set based on a blend of the local rate and a national rate; and 5) Minimum Increase, in which the M+C per capita rate was set based on a minimum increase from the previous year?s rate.
[15] Although the MMA defined the minimum percentage increase as the greater of 2 percent or the growth in national per capita Medicare spending, the DRA no longer provides for the 2 percent minimum update (CMS, 2009).
[16] Currently, an additional budget neutrality adjustment factor is applied to account for the effect of health risk adjustment. This adjustment will be phased out in 2010.
[17] For 2009, the national weights applied to the statutory and plan-bid components are 79.2 percent and 20.8 percent.
[18] Beneficiaries enrolling in these plans would not pay any additional premium beyond the Part B premium, which is paid by both FFS beneficiaries and MA enrollees.
[19] Studies have shown that the absence of network requirements was one of the major factors that made PFFS plans so attractive to MA organizations and enrollees during the first few years of the program (Gold and Peterson, 2006).
[20] This figure is close to the Federal Poverty guideline for individuals ($10,210 in 2007).
[21] This income range is comparable to individuals with incomes that are between 100 percent and 300 percent of the Federal Poverty guideline ($10,210 to $20,630 in 2007).
[22] This pattern has continued in 2009. For example, MedPAC has estimated that ?on average, 2009 MA benchmarks will be 118 percent of spending in Medicare?s traditional FFS program, bids will be 102 percent of FFS spending, and payments will be 114 percent of FFS spending? (MedPAC, 2009a).
[23] CBO?s baseline estimates for Medicare Advantage include projected spending from the stabilization fund for regional PPOs and for certain demonstration programs.
[24] Once they have been determined, MA payments are not modified based on differences that are identified between the plans? projected and actual expenses.
[25] In theory, Medicare has been more successful in achieving a model of managed competition than commercial plans because it primarily relies on private purchasers (rather than employer groups), offers multiple plan choices, and provides fixed contributions toward the cost of coverage (through monthly capitation payments to plans).
[26] For example, although private MA plans have a theoretical advantage in that they do not face the same political obstacles that affect the traditional program, with the exception of the group and staff model HMOs, they generally have not exhibited significant differences in care delivery due to market obstacles (because providers have considerable market power in many areas).
[27] By comparison, the Medicare Savings Program offers direct assistance (e.g., with premiums, deductibles, and/or coinsurance) to beneficiaries who meet the requirements for Qualified Medicare Beneficiaries (QMBs), Specified Low-Income Medicare Beneficiaries (SLMBs), and Qualifying Individuals (1) (QI-1s).
[28] Plans could also potentially receive additional payments without a relationship to outcomes for providing other services that benefit the Medicare program, such as offering coverage to a broad geographic area that includes both urban and rural counties (Berenson and Dowd, 2008).
[29] As discussed earlier, the benchmarks for regional MA plans are based on a combination of the average administered county-level benchmarks and the average bids submitted by plans.
[30] The MMA directs that the Secretary has authority to negotiate monthly bid amounts with plans. However, it is not clear to what extent this is currently occurring, or what improvements could potentially be made in the process.
[31] Another potential competitive bidding approach would involve allowing plans to submit bids, and then buying the benefit package from the lowest cost plans in each county. Under this scenario, competitive bidding would offer an ?opportunity to recalibrate the government?s cost of the entitlement to the cost of the most efficient health plan in each market (either traditional Medicare or a private plan) rather than the cost of the traditional program nationally? (Berenson and Dowd, 2008).
[32] It is possible that Congress may repeal the CCA demonstration (Section 1860C-1) before it begins. For example, the House Tri-Committee Health Reform Discussion Draft included such a proposal (House Committees, 2009).
[33] For example, MedPAC has recently suggested that a blend of 75 percent local FFS cost and 25 percent national weighted average FFS cost would more closely approximate current bidding patterns (MedPAC, 2009b).