U.S. Department of Health and Human Services In Collaboration with the U.S. Department of Labor
This report is available on the Internet at:http://aspe.hhs.gov/health/reports/2011/LGHPstudy/
Printer friendly version in PDF format (8 pages)Free PDF reader 
Currently, the only versions available for these reports are the PDF versions.
- Employer Self-Insurance Decisions and the Implications of the Affordable Care Act (ACA) (180 PDF pages)
- Large Group Health Plans Study (26 PDF pages)
Contents
Summary Report of Research Findings
Study of the Large Group Market
- Why Do Employers Self-Insure?
- Characteristics of Employers
- Analysis of Market Issues
- Effect of the Affordable Care Act Reforms on Adverse Selection and Encouragement for Small and Midsize Firms to Self-Insure
- Data Sources and Limitations
Summary Report of Research Findings
The majority of Americans receive health care coverage through their place of employment. Employers generally choose between two methods of funding when they sponsor a health plan on behalf of their employees. The first method is to fully-insure their plan by purchasing an insurance product through an insurance carrier. The second method is to self-insure the plan, where the employer agrees to take on the financial risk of paying for its employees claims expenses.
Section 1254 of the Patient Protection and Affordable Care Act (P.L. 111-148, the Affordable Care Act), requires the Secretary of Health and Human Services to provide a report to Congress that 1) compares the characteristics of fully-insured and self-insured employers (including industry, size, and other characteristics as determined appropriate by the Secretary), their health plan benefits, financial solvency, capital reserve levels, and the risks of becoming insolvent, and 2) determines the extent to which new insurance market reforms are likely to cause adverse selection in the large group market or to encourage small and midsize employers to self-insure. To fulfill this requirement, the Department of Health and Human Services (HHS), in collaboration with the Department of Labor (DOL), engaged the RAND Corporation and Deloitte Financial Advisory Services LLP to address the questions raised in section 1254. This summary provides highlights of this research; additional details can be found in the final reports from the contractors.
[ Go to Contents ]
Study of the Large Group Market
Deloitte Financial Advisory Services LLP (Deloitte FAS) analyzed the differences between the characteristics of firms that choose to self-insure and those that choose to fully-insure their group health plans, and the factors that appear to influence the decision to select a particular method of funding health plans. A separate study, conducted by RAND, was designed to understand the factors that motivate employers decisions to self-insure and how incentives might change after the Affordable Care Act takes full effect. In addition, RAND assessed the consequences of self-insurance on benefit design, the probability of claims denial, financial risk, and recourse options in the event of a denied claim.
Why
Self-insured firms pay for their workers health care costs directly and bear the risk associated with the year-to-year fluctuations in health care expenditures. Self-insured employers can mitigate some of the risk by purchasing stop-loss insurance, a type of reinsurance for self-insured employers.[1] In contrast, fully-insured firms pay a fixed premium per enrollee to a health insurance issuer with the health insurance issuer bearing the risk for paying claims.
Self-insurance offers a variety of potential advantages to employers, including:
- Autonomy, control, and flexibility over the plan design, including exemption from state mandated benefit requirements;
- Lower administrative services costs than would be charged by a commercial carrier;
- More timely and complete access to data on health claims to help make more informed decisions about the design of their health plan;
- Ease of altering their contract with a third party administrator (TPA) or stop-loss insurer without affecting their employees choice of providers;
- Improved cash flow generated by keeping funds in-house until needed for payment of claims; and
- Avoidance of state insurance premium taxes.
Self-insurance also has potential disadvantages relative to the purchase of a fully-insured product, including:
- Financial risk of unexpectedly large claims;
- Regulatory compliance, which is easier with a fully-insured plan.
Characteristics
Size
Larger firms are much more likely to offer a self-insured plan than are smaller firms. Self-insurance is riskier for smaller firms because small firms have fewer employees over whom to spread the risk of costly claims. Based on 2009 data from the Medical Expenditure Panel Survey, Institutional Component (MEPS-IC), 82 percent of large firms (500 or more employees) offered at least one self-insured plan compared to 13 percent of small firms (under 100 employees). As shown by Figure S-1, over the period from 2002 to 2009, there has been a trend toward self-insurance among larger firms (increasing from 77 percent to 82 percent), while remaining flat for smaller firms (13 percent).
Percent of Private-Sector Establishments Offering Health Insurance That Self-Insure at Least One Plan (Figure S-1) 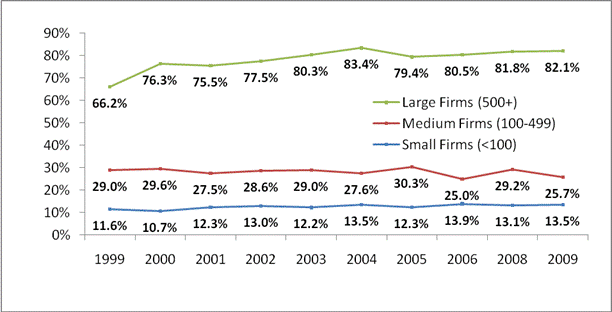 DSource: HHS analysis of data from the Medical Expenditure Panel Survey Insurance Component.
DSource: HHS analysis of data from the Medical Expenditure Panel Survey Insurance Component.
Industry
RAND and Deloitte FAS each analyzed the likelihood of self-insuring by industry. According to Deloitte FASs analysis of the Form 5500 data[2], controlling for plan size, employers in industries that appear to be more likely to self-insure are those in agriculture, mining, construction, manufacturing, transportation, utilities, and finance/insurance/real estate. Less likely are those in communications and information, wholesale trade, retail trade, and services. RANDs analysis of Kaiser/HRET data found that, when not controlling for firm size, the rate of self-insurance is higher among firms in healthcare, manufacturing, transportation/utilities/communication while they are lower in retail and the agriculture/mining/construction industries. Both the Deloitte FAS and RAND analyses indicate that the manufacturing industry is more likely to self-insure, and the retail industry is less likely to self-insure, but many other industries appear to be more likely to self-insure in one analysis but less likely in the other.
Health Plan Benefits
RAND researchers used information on copayments, deductibles, and other out-of-pocket payments to measure the relative generosity of health plans. Little difference in plan generosity between self- and fully-insured plans is found when comparing plans of the same size (2-199, 200-999, 1000+ employees), of the same type (health maintenance organization (HMO), high deductible health plans (HDHP), point of service (POS), and preferred provider organizations (PPO)). In unadjusted analyses, RAND found that self-insured plans offered by small and medium sized firms covered approximately the same proportion of expenses as fully-insured plans, while the proportion of expenses covered by self-insured plans offered by large employers was slightly lower (by 1.7 percentage points or less, depending on plan type) than for fully-insured plans. In adjusted analysis, the study finds no statistically significant differences in plan generosity between self-insured and fully-insured POS or HDHP plans. Among HMO plans, the analysis finds that self-insured plans have statistically significant higher out-of-pocket payments compared to fully-insured plans and found the opposite among PPO plans, where self-insured plans had lower out-of-pocket payments. The differences for both HMO and PPO plans, however, are small in magnitude. The research concludes with no evidence of systematically lower or higher out-of-pocket payments at self-insured firms compared with fully-insured firms. The analysis did not consider the extent to which self-insured plans covered more (or fewer) benefits than fully-insured plans.
Financial Solvency
The Deloitte FAS analysis compared the financial health of fully-insured, self-insured and mixed-funded companies by using three financial measures: the Altman Z score; cash from operations over total debt; and operating income over total debt.[3] The Altman Z score is a composite index used to measure the risk of bankruptcy. Based on this measure, there does not appear to be a systematic relationship between financial health and the employers choice of health plan funding mechanism. Similarly, the cash from operations over debt and operating income measures also suggest comparable financial health across funding types. The analysis does suggest that companies that appear the least financially healthy by these measures (the lowest 25% on each measure) are more likely to be fully-insured than self-insured or mixed-funded.
[ Go to Contents ]
Analysis
Premiums
For fully-insured employers, the premium represents the amount per member per month that the employer must pay the health insurer to cover the health care claims of the employee. Premiums for self-insured plans are estimated, and the methods for estimating premiums vary. As such, it is difficult to directly compare premiums between fully and self-insured plans. Despite these limitations, RAND analyzed differences in reported premiums for self and fully-insured plans. The researchers observe similar premiums across self and fully-insured health plans for most firm sizes and plan types (HDHP, POS, and PPO). However, they find that HMO premiums for self-funded employers are slightly higher than for those purchasing fully-insured products.
Claim Denial Rates
There is no data source that provides systematic, nationally representative data on denial rates for self-insured and fully-insured plans. RAND was able to obtain data from one firm, athenahealth, which in turn obtained data from 11 plans that offer fully-insured products and also administer self-funded products as a TPA. The fragmentary data from this limited set of plans suggests that claim denial rates are similar in the two types of products. This evidence is consistent with the qualitative findings from discussions with stakeholders, indicating that they did not experience any differences in denial rates between self-insured and fully-insured plans.
Plan Benefit Fluctuations (A Potential Measure of Scaled Back Plans During Economic Downturns)
As measured by plan actuarial values, the year-to-year changes in the overall generosity of benefits between self- and fully-insured plans were not significantly different. However, the analysis was limited in that the changes were observed over a short time frame (2007-2010).
The Impact of Limited Recourse Options for Consumers
Both self-insured and fully-insured plans are subject to ERISA requirements for internal claims appeals, with fully-insured plans also subject to any state appeal requirements. Under the Affordable Care Act, both plan funding types are subject to new standards for internal appeals, increasing consumer protections.
ERISA does not require any particular type of external review or independent medical review to be available to consumers who experience adverse claims decisions, and ERISA preempts states from requiring external review options for consumers in self-insured plans. For fully-insured plans, states may impose external review requirements, and all but six have done so in varying degrees. The implementation of the Affordable Care Act requires that an external review be available to consumers in all states for fully-insured and self-insured plans. This requirement applies to all non-grandfathered plans, irrespective of funding status.
The Affordable Care Act narrows the gap that had emerged in recent decades between the external review rights of consumers in self-insured and fully-insured plans. As grandfathered status becomes less common over time, the review processes will be more similar. The remaining differences will stem from any differences between state programs that apply to fully-insured plans and the federal programs that cover the self-insured.
Potential Conflicts of Interests
A potential conflict of interest arises in health insurance claims adjudication because the same insurance company that decides which claims to pay is also financially responsible for making the payments. Similarly, there may be conflicts of interest in the administration of self-insured plans. To assess the extent to which conflicts of interest operate differently in self-insured and fully-insured plans, RAND researchers held discussions with stakeholders including consumer groups, self-insured companies, third party administrators (TPAs), stop loss insurers, and experts on self-insurance. Among the stakeholders interviewed, there was no perception of a greater conflict of interest in claims adjudication among self-insured than among fully-insured plans. Insurance companies reported no difference in their rules for initial determinations of claims from fully-insured plans versus claims processed through an Administrative Services Only (ASO) contract handling self-insured plans. Employers that changed coverage between self-insured and fully-insured similarly reported no systematic differences in the handling of claims. While the prospect of lower benefit payments might appear to result in a greater incentive to deny claims for self-insured plans than fully-insured plans, because the financial benefit accrues directly to the employer, stakeholders noted that the financial incentives to deny medical claims might be smaller for self-insured plans for two reasons. First, self-insured employers are generally willing to invest in medical spending because of their financial stake in the health and well-being of their employees and in employee satisfaction. Second, although the self-insured plan sponsor often is the ultimate decision maker, industry experts indicate that employers rarely dispute claims that a TPA has approved. Further, in accordance with an NAIC model act, contracts with TPAs rarely (if ever) tie payment to any metric concerning claims denials.
Administrative Costs
There were insufficient data to determine the effect, if any, of the specific funding mechanism on plan administrative costs.
[ Go to Contents ]
Effect of the Affordable Care Act Reforms on Adverse Selection and Encouragement for
The RAND research findings suggest that there will be little change in self-insurance rates after the Affordable Care Acts insurance market reforms are fully implemented in 2014, although the results are sensitive to the assumptions made about the availability of attractively priced reinsurance.
Community rating for small employers both inside and outside the Exchange beginning in 2014 will increase the incentives for employers with low-risk employees to switch from being fully-insured to self-insurance.[4] If employers with healthy employees opt for self-insurance and leave employers with sicker employees in the community-rated pool, this may lead to adverse selection and increases in premiums for those in the community-rated group. However, the extent of this shift is expected to be limited because self-insurance entails much greater financial risks than full insurance, and these greater risks will likely discourage many small employers from switching to self-insurance.
The extent to which small employers move to self-insurance depends on the reinsurance market. Because there is little data available, and after consultation with industry experts, the researchers believe that attractively-priced stop-loss with low attachment points is not currently widely available for small employers. It is unclear whether the reinsurance market will change substantially, although there are some anecdotal reports that reinsurance with relatively low attachment points is becoming more widely available. If the reinsurance market were to change, and attractively-priced reinsurance providing coverage beginning at low levels of stop-loss became widely available, then there would likely be substantial movement of small employers to self-insurance. A similar shift would likely occur in the current market if such a product existed today, although the incentives to move to self-insurance for small employers with younger and healthier workers are expected to be somewhat greater after 2014. However, HHS cannot predict the impact of the Affordable Care Act on the reinsurance market since it was not studied in the RAND report.
These results highlight the importance of closely monitoring the availability and pricing of reinsurance, and closely monitoring decisions made by small employers to self-insure.
[ Go to Contents ]
Data
Deloitte FAS analyzed the information health plan sponsors or administrators provided on the Form 5500 for the plan years 2000 to 2008 as the primary data source for their report. Private sector health plans with 100 or more participants are required to annually file a Form 5500 with the Department of Labor; public sector plans and most employers with fewer than 100 employees are excluded. This form captures information such as the number of participants covered by the plan, insurance expenses, whether the plan is at least partially self-insured, and, for a subset of plans that have established a trust, plan expenses and participant contributions. To obtain greater information about the firms sponsoring the plans, including their characteristics and financial health, Deloitte FAS matched the Form 5500 data to external financial data captured in the Capital IQ data base. There are limitations to the Form 5500 data, including incomplete or inconsistent information.
RAND analyzed data on plan benefits from the Kaiser Family Foundation/Health Research and Educational Trust Annual Survey of Employer Benefits. As noted above, data on claims denial and premiums are fragmentary. RANDs analysis of claims denials used data from 11 plans that offer fully-insured products and also administer self-funded products as a TPA, providing a limited comparison on claims denials between the two groups. Additionally, the COMPARE model RAND used cannot capture all of the factors that influence firms decisions. For example, the model cannot incorporate issues such as employers private knowledge about employees health status. The model is also constrained by data limitations, such as lack of information on stop-loss policies and the absence of data linking employees, employers, and health expenditures. Additional information on the datasets and limitations can be found in the source reports.
[ Go to Contents ]
Endnotes
[1] In a typical stop-loss arrangement, the reinsurer agrees to pay a proportion of medical expenses (for example, 80%) if claims for an individual are above a threshold, or attachment point (for example, $75,000). Some self-insured employers also purchase aggregate reinsurance, in which the reinsurer agrees to pay claims if aggregate medical expenses for the group are greater than some percentage (for example, 125%) of the expected expenditures for the group.
[2] The Form 5500, Annual Return/Report of Employee Benefit Plan, is an Internal Revenue document used to report information concerning employee benefit plans. Any administrator or sponsor of an employee benefit plan subject to ERISA must file information about each benefit plan every year (pursuant to Code section 6058 and ERISA sections 104 and 4065). Form 5500 is an important compliance, research, and disclosure tool for the Department of Labor, a disclosure document for plan participants and beneficiaries, and a source of information and data for use by other Federal agencies, Congress, and the private sector in assessing employee benefit, tax, and economic trends and policies. The Form 5500 Series is part of ERISA's overall reporting and disclosure framework, which is intended to assure that employee benefit plans are operated and managed in accordance with certain prescribed standards and that participants and beneficiaries, as well as regulators, are provided or have access to sufficient information to protect the rights and benefits of participants and beneficiaries under employee benefit plans.
[3] Mixed-funded companies are those that offer both self-insured and fully-insured plans.
[4] Under pure community rating, premiums are the same for all employers. Community rating is a method of setting insurance premiums that ignores any differences in expected costs among insured groups or people.
[ Go to Contents ]
